Nurse Burnout and Employee Engagement: What Hospitals Must Fix in 2026


 Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.
Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.

This article is for CHROs, HR Operations Directors, and hospital HR leaders managing clinical and nursing workforces. It explains why nurse burnout and employee engagement are the same problem — and why treating them separately means neither improves.
Three evidence-based fixes address the root causes: transforming nurse onboarding with pre-boarding and role-specific pathways; engaging shift workers and night nurses through mobile-first tools; and building a structured first-90-days framework with 30-60-90 check-ins and peer buddy systems.
Sustained engagement beyond the first 90 days requires career development visibility, flexible scheduling, and manager coaching on early burnout recognition. Hospitals applying these engagement strategies consistently report lower burnout rates, reduced first-year departures, and measurable improvements in patient safety outcomes.
By 2026, hospitals will lose one in five nurses to burnout-related turnover. At $46,000 to $64,000 per departure, a mid-market system losing 40 nurses a year is quietly burning through $2.5 million in its operating budget. Not from a crisis or blackswan event such as COVID-19 but owing to a preventable failure to keep the nurses engaged.
Yes, nurse burnout and employee engagement are not separate problems. They don't require separate interventions either. Disengaged nurses burn out faster. Burned-out nurses disengage further. Hospitals treating these as two distinct HR workstreams tend to improve neither.
The good news is that three targeted fixes can start reversing this cycle within weeks. And all three sit squarely within HR's control.
Nurse Engagement Gap You Can't Ignore
The NSI Nursing Solutions 2024 National Health Care Retention Report put hospital turnover at 22.7% and nursing turnover at 27.1%. Those aren't just headcount numbers. For mid-market healthcare systems, they represent a structural budget burden — driven not by external forces, but by disengagement that accumulates shift by shift, unit by unit.
Burnout's Ripple Effect on Patient Care
We have already discussed the financial burden of nurse dis-engagement. The clinical stakes are equally serious. Research from Press Ganey shows that hospitals in the top quartile for staff engagement experience 41% fewer patient safety incidents.
So, burned-out nurses make more errors and leave faster. But they take with them the institutional knowledge and patient relationships that no orientation programme can quickly replace.
Why Nurse Engagement Fails
According to Gallup's workplace research, only 23% of employees globally feel engaged at work. In healthcare, the picture is more acute.
Burnout prevalence runs high across nursing specialties, and a significant portion of clinical staff report moderate-to-severe exhaustion. Disengaged nurses are far more likely to leave within 6 to 12 months.
Most hospitals are short on the right infrastructure to hire, engage, and retain registered nurses. But these three patterns show up most consistently, and they all have a fix.
The Deskless Disconnect
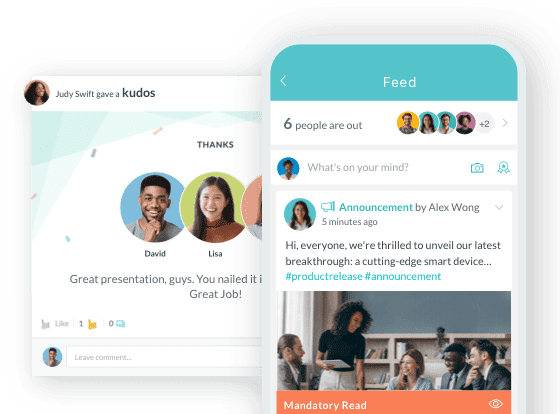
Approximately 70% of nurses are deskless workers with no reliable access to email or desktop systems during their shifts. Traditional healthcare employee engagement tools such as intranet portals, email-based surveys, desktop recognition platforms, etc. miss the majority of clinical staff entirely.
Night and weekend shift nurses operate in a near-complete information vacuum: no company updates, no real-time recognition, no signal that leadership is aware they exist.
One-Size-Fits-All Onboarding
An ED nurse sitting through the same orientation as an administrative coordinator creates early disengagement before a single shift begins.
When new nurses can't find role-specific information in their first week, they default to asking already-stretched colleagues. That further burdens the team.
It also signals to the new nurse that the organization wasn't ready for them. Early disengagement in healthcare is rarely about compensation. It's almost always about an impersonal start.
Communication Black Holes
Delayed feedback loops, no real-time recognition for shift workers, and the near-total absence of peer connection across shifts are the very structural conditions that have the capability to erode employee engagement and mental health. Until a resignation letter or email lands on HR’s desk, making the problem visible.
And by then, it's probably too late.
You need to take action that will fix these challenges.
Three Fixes That Actually Work
Fix #1: Transform Your Nurse Onboarding
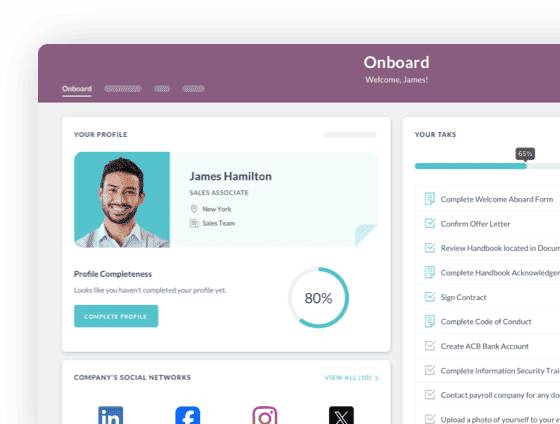
The single most underrated engagement lever in healthcare HR is what happens in the first 90 days. And ironically, it is also — what doesn't happen. Most hospitals rely on a generic orientation and a paper-heavy compliance checklist. The manager is notified of the new hire's start date 48 hours before arrival.
The fix begins before day 1. During the pre-boarding.
Sending welcome content, completing I-9 paperwork digitally, and giving new nurses early access to shift schedules — all these make the new hire get excited about their new job before the first shift starts.
Research published in BMC Nursing shows that nurses who feel prepared on day 1 are significantly more likely to stay engaged and adapt to organisational culture faster.
Nurse onboarding best practices in 2026 require role-specific clinical checklists.
An ICU nurse and a Med-Surg nurse do not need the same path.
They also require competency tracking with automated manager reminders.
Mobile-first document access matters too. For staff who will never sit at a desktop. Hospitals using automated onboarding complete the process up to 3x faster. The engagement impact through the first year is equally significant.
Fix #2: Engage Shift Workers and Night Nurses
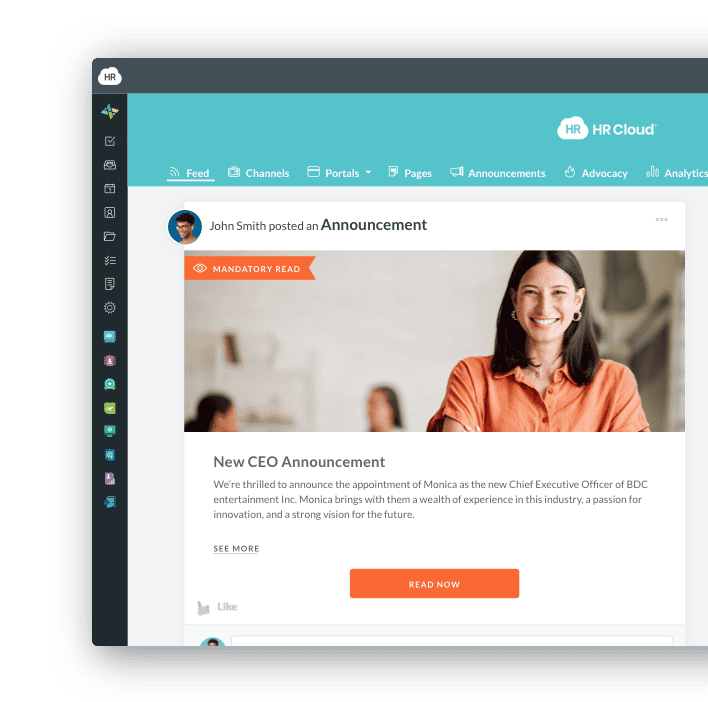
Here's what I know about night shift nurses: they are the most disengaged population in most hospitals. The engagement tools most hospitals use were built for the other half of the workforce. A recognition post that requires a desktop login, published on a Tuesday afternoon, doesn't reach a nurse finishing a night shift at 7 a.m. on a Saturday. It simply doesn't exist for her.
Shift worker engagement means meeting clinical staff where they actually are — on their phones, between patient rooms, in the ten minutes before a handoff. Mobile employee apps with shift-specific news feeds and instant peer-to-peer recognition are not feature preferences. SMS-based pulse surveys of two or three questions, mobile-native, are not a nice addition. They are the baseline for reaching 70% of your clinical workforce.
The burnout symptoms that predict resignation — chronic fatigue, withdrawal from the team, declining survey participation — show up in engagement data weeks before exit interviews reveal them. But only if your tools actually reach the people experiencing them. A recognition feed night nurses can access at 2 a.m. is not a nice-to-have. It's an early warning system.
Fix #3: Master the First 90 Days
40% of nurse turnover happens within the first six months, and the engagement trajectory set in the first 90 days predicts most of it. Fix #1 addresses the mechanics of onboarding. This fix addresses what comes after — the ongoing relationship between a nurse and their manager, their peers, and their unit.
That's why a structured first-90-days framework matters — not as a wellbeing initiative, but as an engagement infrastructure. The 30-60-90 check-in framework is the structural response.
At day 30, the manager conversation is about belonging and early wins. Does this nurse feel seen? Are expectations clear?
At day 60, the focus shifts to integration. Are skill gaps emerging? Is peer connection forming?
At day 90, the it’s all about understanding the trajectory. Does this nurse see a future here?
Automated reminders ensure these conversations happen across all managers, not just the naturally attentive ones.
Peer buddy systems — matched by shift and specialty, not just department — are the other lever. Research in PubMed Central shows that nurses with strong peer connections are significantly less likely to experience burnout. A structured buddy programme doesn't require a large investment. It requires intentional matching and a platform where those connections can continue digitally across shifts.
What Sustains Nurse Engagement Beyond the First 90 Days
The three fixes address the most burning problem.
Sustaining that engagement requires a longer view. Nurse engagement strategies that hold over time combine three things.
-
Career development visibility gives nurses a path forward, not just a current role.
-
Flexible scheduling — specifically the ability to manage shift swaps — gives nurses genuine agency.
-
Manager training on early burnout recognition means someone is watching for disengagement signals before they become resignation letters.
The ROI of investing in sustained engagement is unambiguous. A 200-bed hospital where nurses feel genuinely engaged — recognised, heard, and growing — doesn't just see lower burnout. It sees better patient outcomes and lower agency staffing spend.
How HR Cloud Supports Hospitals in 2026
HR Cloud was built for the workforce healthcare organizations actually have — not the office-based workforce most HR software assumes.
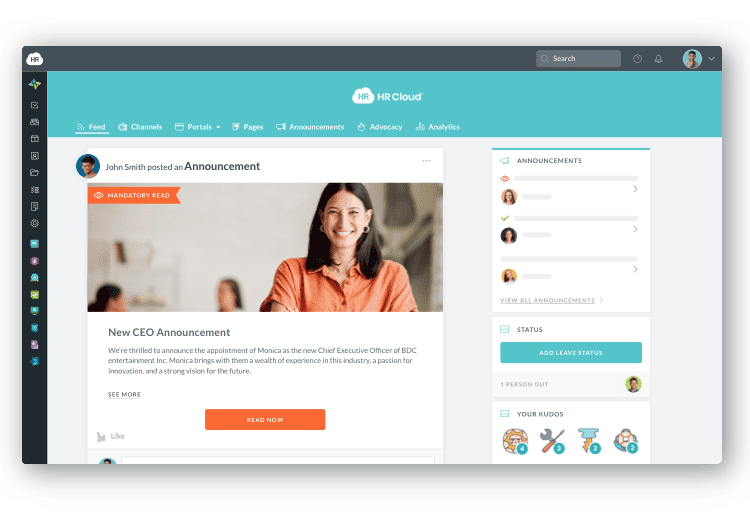
The Workmates engagement module delivers mobile-first peer recognition, pulse surveys, and team communication in a single app. It's accessible from any device, on any shift, including nights and weekends.
The onboarding module automates pre-boarding workflows, role-specific checklists, I-9 compliance, and manager check-in reminders in one connected system.
Behavioral Progression Inc. is a behavioural health organisation facing the challenge of engaging and retaining clinical staff in a high-turnover, compliance-heavy environment.
After implementing HR Cloud, they
-
reduced new hire questions by 60%
-
cut onboarding from 4 weeks to 2.5 weeks
-
increased employee engagement to 20%
-
improved six-month retention by 10%
The best part is that these outcomes compound.
Engaged clinical staff ask fewer questions, complete onboarding faster, and stay long enough to build the patient relationships that define quality care.
Analytics connect engagement data — recognition activity, survey participation, check-in completion — to clinical and business outcomes. This gives HR leaders the evidence necessary to have the necessary financial conversation about engagement investment.
See how HR Cloud's healthcare engagement software works for shift-based clinical environments, or explore the full Behavioral Progression case study.
Metrics That Tell You Whether It's Working
If you don’t measure, how will you know if your effort is fruitful? The engagement signals worth tracking fall into three categories:
-
Leading indicators tell you whether nurses are actively engaged right now. These include onboarding completion rates, 30/60/90-day check-in completion by manager, pulse survey participation by shift, and recognition activity sent and received per unit. These are the early signals. If they're moving in the right direction, retention outcomes tend to follow.
-
Lagging indicators confirm whether engagement translated into stability. These are your 90-day retention rate, 12-month voluntary turnover by department, and time-to-productivity measured through competency validation. They confirm what happened — but they're too slow to be actionable on their own.
-
Outcome metrics make the business case: patient satisfaction scores, safety incident rates, absenteeism by unit, and eNPS. Hospitals tracking engagement metrics alongside clinical outcomes — not in separate dashboards — are the ones that move both.
The Fix Is Within Reach. What is the Delay Then?
The nurse burnout crisis is real, measurable, and expensive. It's also quite preventable.
Better onboarding, mobile-first shift worker engagement, and a structured first 90 days don't require major structural redesign. Just systems built for the workforce you actually have.
But remember that you need to close the feedback loop for any change to really happen.
When nurses tell you night shift workers feel invisible, listen to them and solve their problems.
When 90 days later your mobile recognition data shows adoption on nights has tripled, know that your fix has worked.
Hospitals that connect "we listened" to "we acted" build the kind of engagement that outlasts any single programme.
FAQs
What is the connection between nurse burnout and employee engagement?
Nurse burnout and employee engagement are directly linked. Chronic workplace stress, heavy workloads, and lack of recognition reduce engagement breeds a group of disengaged nurses, who are significantly more likely to experience accelerated burnout. Hospitals that improve engagement through structured onboarding, mobile recognition, and consistent manager check-ins see measurable reductions in both burnout rates and voluntary turnover.
How can hospitals reduce nurse burnout in 2026?
Hospitals can reduce nurse burnout through three core interventions: transforming onboarding with pre-boarding and structured 90-day plans; engaging shift workers through mobile-first communication and real-time recognition tools; and implementing pulse surveys that reach all shifts, not just day-shift staff. Healthcare onboarding software and mobile engagement platforms enable these strategies at scale, shifting the approach from reactive to preventive.
What are the best nurse retention strategies for 2026?
The most effective nurse retention strategies in 2026 combine structured onboarding, 30-60-90 day check-in frameworks, peer buddy systems matched by shift and specialty, mobile recognition programmes, career development pathways, and data-driven early warning systems to identify at-risk staff. Hospitals consistently applying these strategies see meaningful reductions in first-year turnover and significant savings in agency staffing costs.
Why do night shift nurses experience higher burnout?
Night shift nurses experience higher burnout due to circadian disruption, social isolation from day-shift leadership, delayed or absent recognition, and limited access to the engagement tools deployed for day-shift staff. Addressing this requires mobile-first engagement infrastructure that functions equally well at 2 a.m. as at 2 p.m. — including shift-specific recognition programmes and manager check-ins that aren't confined to business hours.
What is the cost of nurse turnover in 2026?
Replacing one registered nurse costs between $46,000 and $64,000, accounting for recruitment, onboarding, training, and productivity loss during vacancy. For a 200-bed hospital with 20% annual nursing turnover, total replacement costs can reach $3.7 to $5.1 million annually. Reducing turnover by 5% through improved engagement and onboarding saves over $1 million per year — before accounting for reduced agency staffing spend.

Keep Reading
New Manager Training Without a Formal L&D Program
Your best individual contributor just got promoted. They know the work cold. They know
The Manager's Role in Employee Retention: What the 2026 Data Shows
If your organization is spending money on engagement surveys, benefits upgrades, and
How to Use AI in HR: Moving From Drafts to Trackable Workflows Across the Full Lifecycle
You're an HR director at a 400-person company. You have three open requisitions, a
Like What You Hear?
We'd love to chat with you more about how HR Cloud® can support your business's HR needs. Book Your Free Demo

Build a Culture of Recognition. Boost Engagement. Guaranteed.
Workmates empowers employees to stay informed, connected, and appreciated—whether they’re on the front line, in the office, or remote. Recognition drives 12x higher engagement.Trusted by industry leaders in every sector




Cut Onboarding Costs by 60%.
Take the confusion and follow-ups out of onboarding with automated workflows, digital forms, and structured portals—so new hires ramp faster 3X quicker.Trusted by industry leaders in every sector