Primary vs Secondary Medical Insurance
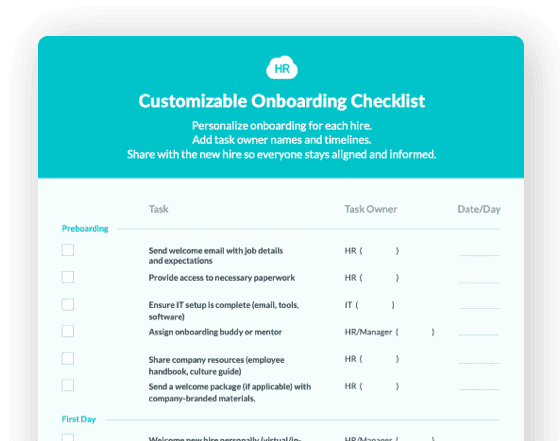
 Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.
Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.

What Is Primary vs Secondary Medical Insurance?
When a person is covered by more than one medical insurance plan, the two plans coordinate their payments using a process called coordination of benefits (COB). The plan that pays first is the primary insurance, and the plan that steps in to cover remaining costs afterward is the secondary insurance.
This coordination exists because two health plans cannot together pay more than the actual cost of a medical service. The primary plan pays its portion according to its own terms, and then the secondary plan may cover some or all of the remaining balance, up to the total cost of care. The patient pays whatever is left after both plans have applied their rules.
For employees, understanding primary versus secondary medical insurance matters most when they are covered by their own employer plan and a spouse's employer plan, when a child is covered by both parents' plans, or when an employee is enrolled in Medicare alongside an employer plan. For HR professionals, correctly communicating how coordination of benefits works is a key part of benefits administration and reduces employee confusion during claims.
HR Cloud's benefits administration platform supports dual-coverage tracking and helps HR teams collect coordination of benefits data during open enrollment so claims are processed correctly from the start.
Key Points
Coordination of benefits follows established rules that determine which plan pays first, and the outcome affects how much the patient ultimately owes.
-
The primary plan always pays first, based on its own deductibles, copays, and coverage rules, without considering what the secondary plan will cover
-
The secondary plan pays after the primary, and it can only cover up to the amount remaining after the primary plan has paid, never more than the total cost of service
-
If the primary plan fully covers a service, the secondary plan pays nothing for that service
-
The most common COB rules are: your own employer plan is primary for yourself; the birthday rule determines primary coverage for a dependent child covered by both parents' plans; Medicare coordination rules depend on employer size and active employment status
-
Not all secondary plans work the same way; some use a "maintenance of benefits" approach while others use a "carve-out" approach, which produce different out-of-pocket amounts
-
Employees must disclose other coverage to their insurer; failure to do so can result in claim denials or retroactive adjustments
Common Primary vs Secondary Insurance Scenarios
Real-world coordination of benefits plays out differently depending on which plans are involved and how they relate to the patient.
|
Scenario |
Primary Insurance |
Secondary Insurance |
|---|---|---|
|
Employee covered by own plan + spouse's plan |
Employee's own employer plan |
Spouse's employer plan |
|
Dependent child, parents married |
Parent whose birthday falls earlier in the year |
Other parent's plan |
|
Dependent child, parents divorced |
Plan of parent with legal responsibility (per court order) |
Other parent's plan |
|
Employee with Medicare, employer size 20+ |
Employer group plan |
Medicare |
|
Employee with Medicare, employer size under 20 |
Medicare |
Employer group plan |
|
Employee covered by COBRA + new employer plan |
New employer plan |
COBRA |
|
Employee with Medicaid + employer group plan |
Employer group plan |
Medicaid |
Best Practices
Getting primary versus secondary insurance right requires clean data, consistent communication, and alignment between your HR team and your benefits carrier.
Collect coordination of benefits information from every employee at enrollment. Your group health plan likely requires you to ask employees whether they or their covered dependents have other medical coverage. Collecting this information consistently and storing it in your HRIS system ensures that your insurer has accurate COB data when processing claims.
Explain the birthday rule to employees before open enrollment closes. Many employees with children covered by two parental plans are not aware of the birthday rule, which states that the parent whose birthday falls earlier in the calendar year (month and day, not year) has the primary plan for the child. Communicating this rule before a claim is submitted prevents frustration when a claim is processed differently than expected.
Train HR and benefits staff on the Medicare secondary payer rules. These rules are governed by federal law, not just plan documents, and the consequences of getting them wrong are significant. According to the Centers for Medicare and Medicaid Services, employers who incorrectly make Medicare primary for an active employee at a company with 20 or more workers can face substantial civil penalties.
Update COB records whenever an employee reports a life event that affects their coverage. Marriage, divorce, a spouse's job change, and a dependent aging off a parent's plan all create changes in primary/secondary designation. Having a clear process for employees to report these changes, and a workflow to update the insurer, prevents months of claims processing errors.
Pitfalls to Avoid
These misunderstandings are common and lead to denied claims, unexpected bills, and employee frustration.
Assuming the secondary plan will cover all remaining costs. Secondary plans also have their own deductibles, coinsurance, and coverage exclusions. An employee who receives a $200 bill after the primary plan pays may expect the secondary plan to cover it entirely, but the secondary plan may apply its own cost-sharing and cover only $120. Setting realistic expectations during enrollment prevents disappointment.
Confusing supplemental insurance with secondary medical insurance. Short-term disability, hospital indemnity, accident policies, and cancer policies are supplemental coverages that pay fixed benefits based on events, not on medical claims. They do not participate in coordination of benefits with a medical plan. An employee who assumes their accident policy will act as secondary medical insurance will be confused when it does not work that way.
Failing to notify the insurer when secondary coverage exists. Most group health plans require employees to disclose other coverage. If an employee does not disclose secondary coverage and the insurer later discovers it, the insurer may retroactively adjust paid claims, creating unexpected liability for the employee.
Mishandling COBRA coordination. When an employee leaves a job and continues coverage on COBRA while also enrolling in a new employer's plan, the new employer's plan is primary and COBRA is secondary. Some employees and HR teams incorrectly assume that COBRA replaces the prior primary designation. This error can delay claim payment or cause incorrect billing.
Industry Applications
Primary versus secondary medical insurance coordination plays out with particular frequency in industries where dual coverage is common among the workforce.
In healthcare, where clinical staff often have spouses in the same or adjacent professions with their own employer-sponsored coverage, dual coverage is widespread. Healthcare HR teams handle high volumes of COB questions during open enrollment and throughout the year when claims are processed unexpectedly. Connecting HR Cloud's benefits administration tools with your group health insurer's COB system ensures that enrollment data and COB designations flow correctly without manual re-entry.
In education, school districts frequently employ both spouses, particularly in smaller communities. When two teachers at the same district are married, COB designation for their children is determined by the birthday rule, and HR needs to communicate this clearly during the district's annual benefits enrollment period each summer.
In manufacturing and construction, where union-negotiated coverage from a Taft-Hartley plan may coexist with a spouse's employer plan, COB rules can involve multi-employer plan documents with complex coordination language. HR teams in these environments benefit from a clear written summary of how the union plan coordinates with other coverage.
Implementation Plan
Managing primary and secondary medical insurance coordination well requires process and data, not just policy knowledge.
Add COB disclosure to your enrollment form. Every employee electing medical coverage should be asked whether any covered family member has other medical insurance. Capture the other insurer's name, group number, and effective date.
Determine and record primary/secondary designations. Using the COB rules that apply to your plan, record which plan is primary and which is secondary for each covered family unit. Store this information in your HRIS or benefits administration system.
Communicate COB rules at enrollment. Provide employees with a plain-language explanation of the birthday rule, Medicare coordination, and the general claims sequence during open enrollment. A one-page reference card is more effective than a dense plan document paragraph.
Set up a life event update process. Create a clear workflow for employees to notify HR when they experience a change that affects their coverage designation, and build in a corresponding step to notify the insurer of the change.
Review COB records annually. At each open enrollment, prompt all employees with dual coverage to confirm whether their secondary plan has changed. Update records before the new plan year begins.
Train HR staff on Medicare coordination. Identify employees who are 65 or older or who have Medicare for any reason, and confirm the correct primary/secondary designation based on employer size and active employment status.
Future Outlook and Trends
Coordination of benefits is becoming more complex as health coverage diversifies. The expansion of individual coverage health reimbursement arrangements (ICHRAs), health sharing ministries, and marketplace plans alongside traditional employer-sponsored coverage is creating new combinations of primary and secondary payers that traditional COB frameworks were not designed to address.
The rise of telehealth benefits purchased as standalone products also creates coordination questions. When an employer sponsors a telemedicine benefit through a third-party provider alongside a traditional group health plan, determining which is primary for a virtual care visit depends on how each plan defines covered services.
Health technology is improving the accuracy and speed of COB processing. Real-time data exchange between insurers, which historically required days or weeks of back-and-forth claims adjudication, is moving toward automated coordination that settles COB in real time at the point of service. When fully implemented, this will significantly reduce the billing confusion that employees experience today.
According to research published by SHRM on employee benefits communication, employees who clearly understand how their health coverage works report higher satisfaction with their benefits package, even when the coverage itself has not changed. Clear COB communication is one of the highest-leverage improvements an HR team can make to benefits satisfaction without changing any plan design.
HR Cloud's benefits administration platform helps organizations build coordination of benefits data collection into enrollment workflows, so your team and your insurer always have the accurate information needed to process claims correctly.
 Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Keep Reading
AI-First HR Infrastructure: The Complete Guide to Building HR That Runs on Intelligence, Not Effort
You bought the AI add-on. You sat through the demos. You approved the budget. And now,
AI Onboarding for Field Workers: Why Compliance Is the Real Test (And How to Pass It)
Approximately 80% of the global workforce is deskless — field workers, frontline staff,
HR Cloud Healthcare Onboarding & Scheduling
You hired a CNA last Thursday. She starts Monday. Between now and then, HR is chasing
Ready to streamline your onboarding process?
Book a demo today and see how HR Cloud can help you create an exceptional experience for your new employees.

