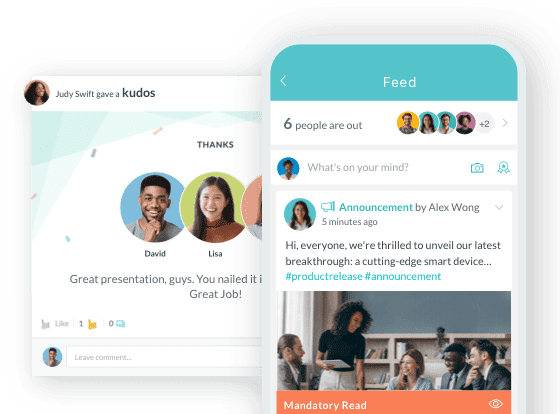
Caregiver no-shows can disrupt patient care, strain schedules, and increase operational costs for home care agencies. This blog explains how HR leaders can reduce missed shifts by improving scheduling transparency, strengthening communication, and setting clear expectations from day one. It highlights practical steps such as automated shift reminders, reliable backup staffing plans, and better caregiver engagement. By creating structured processes and stronger accountability, agencies can maintain consistent staffing, improve caregiver reliability, and deliver more dependable care to patients.
How to Reduce Caregiver No-Shows in Home Care

- Introduction
- The True Cost of Caregiver No-Shows
- Why Caregivers Don't Show Up
- How Structured Onboarding Reduces No-Shows
- Recognition and Engagement Strategies
- Optimizing Scheduling to Prevent No-Shows
- Real-Time Communication Tools
- Measuring and Improving
- Implementation Timeline: From Assessment to Results
- Creating a Culture of Reliability
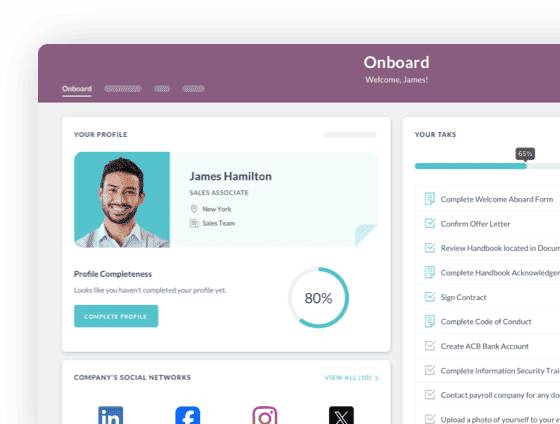

 Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.
Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.

Caregiver no-shows create costly operational disruptions in home care agencies, but agencies can reduce them through structured onboarding, recognition systems, flexible scheduling, and real-time communication tools. Organizations using automated onboarding platforms and employee engagement solutions see measurable improvements in attendance reliability and overall workforce stability.
Key Takeaways
-
Caregiver turnover reached 75% in 2025, with replacement costs averaging $2,600 per caregiver — making attendance reliability essential for financial sustainability
-
59% of home care agencies report ongoing caregiver shortages, making every scheduled shift critical for meeting client commitments and maintaining service quality
-
Structured onboarding processes with automated checklists, chained task workflows, and scheduled check-ins at 7, 30, 60, and 90 days reduce early attrition, which directly correlates with fewer no-shows
-
Recognition and rewards programs improve caregiver engagement and shift reliability when tied to specific behaviors like perfect attendance and paired with meaningful incentives
-
Automated scheduling with mobile access, geolocation-verified time tracking, and caregiver preference integration helps caregivers manage commitments more effectively
-
Real-time communication channels with searchable message history reduce misunderstandings that lead to missed shifts
-
Quick wins like digital shift confirmations reduce no-shows by 15-25% within weeks, while systematic interventions deliver 30-40% improvement within months
-
Measuring key metrics including no-show rates by caregiver tenure, shift type, and day of week enables data-driven optimization
Introduction
Sarah pulled up to her client's home at 6:45 AM, expecting to hand off the morning shift to Amanda, the scheduled caregiver. By 7:15 AM, after three unanswered calls, Sarah realized Amanda wasn't coming. Again. She'd have to cancel her afternoon appointments to cover the shift — the third time this month she'd rearranged her life to fill gaps left by no-shows.
This scenario plays out thousands of times daily across home care agencies nationwide. Caregiver no-shows aren't just scheduling inconveniences. They disrupt client care continuity, burn out reliable staff who scramble to cover gaps, damage agency reputations in competitive markets, and drain resources that could fuel growth. With 75% caregiver turnover and replacement costs hitting $2,600 per hire, agencies can't afford to treat attendance problems as an inevitable cost of doing business.
The good news? No-shows aren't random occurrences. They're symptoms of deeper workforce management challenges — and they respond to systematic solutions. Agencies that address root causes through better onboarding processes, employee engagement strategies, automated scheduling systems, and real-time communication see measurable declines in missed shifts and improvements in overall workforce stability.
Home care agencies report that client and caregiver scheduling emerged as the top system priority in 2025, with 51% of providers focusing on optimizing shift management to reduce operational disruptions. This shift in focus reflects the industry's recognition that attendance reliability directly impacts both client satisfaction and financial performance.
The True Cost of Caregiver No-Shows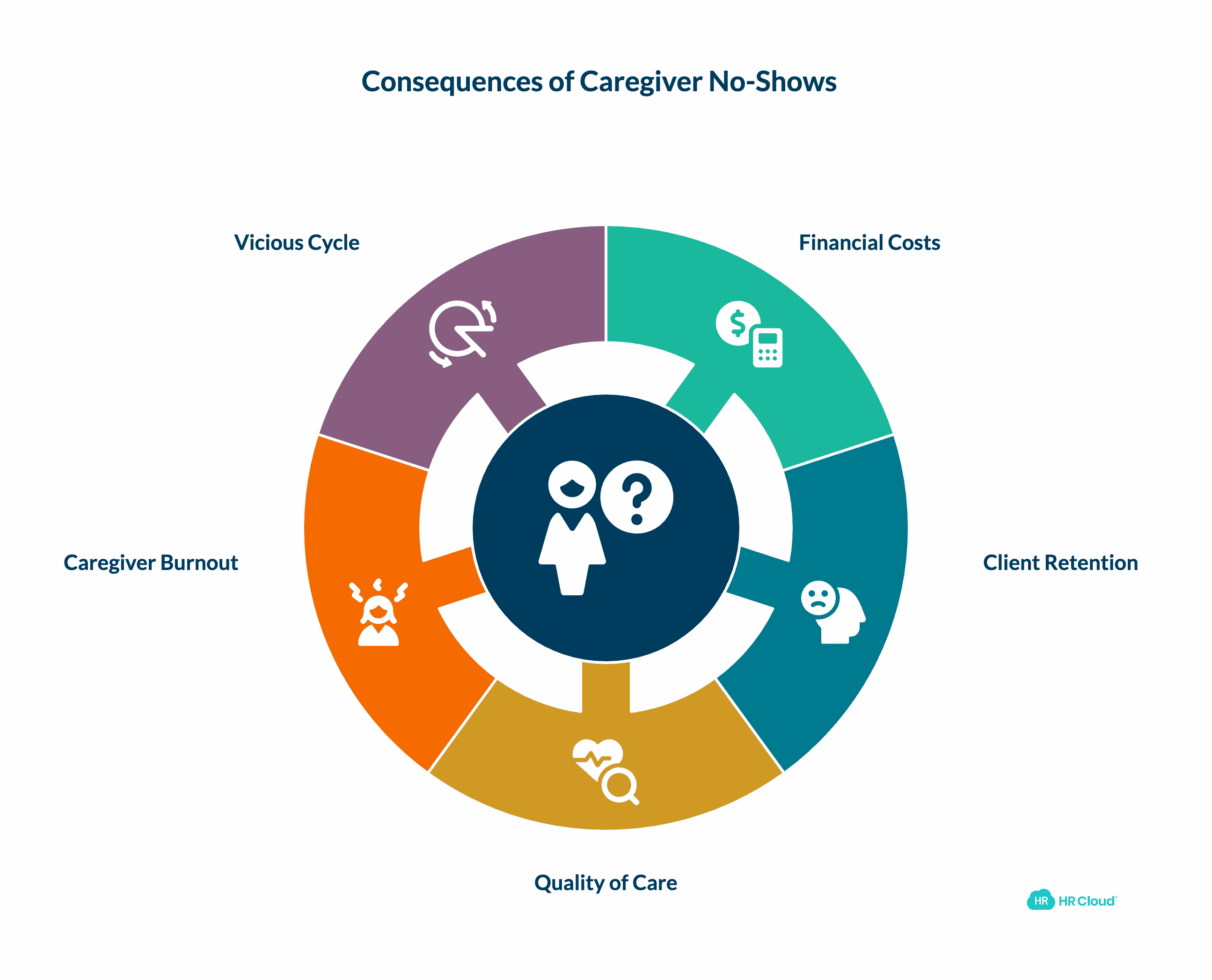
When a caregiver doesn't show up for a scheduled shift, the immediate scramble to find coverage masks much larger operational costs.
First, there's the direct financial impact. Office staff spend hours making emergency calls, shuffling schedules, and sometimes authorizing premium pay to secure last-minute replacements. Agencies working with backup caregiver pools often pay 20-30% higher hourly rates for emergency coverage. When no replacement can be found, agencies may need to refund services or risk regulatory compliance issues.
Client retention takes a hit too. Home care clients develop relationships with their assigned caregivers. When those caregivers repeatedly fail to show up, clients experience stress and inconsistency in their daily routines. According to the 2025 Activated Insights Benchmarking Report, home care client turnover dropped to 45.5% among agencies that improved communication and consistency — suggesting that reliability directly influences client satisfaction and retention.
The home care industry's shift toward value-based care models makes attendance reliability even more critical. Agencies increasingly compete on quality metrics and client outcomes rather than just price. Consistent caregiver presence enables better chronic disease management, medication adherence monitoring, and relationship-based care that improves health outcomes. No-shows disrupt this continuity and undermine quality-focused competitive positioning.
Your reliable caregivers bear the heaviest burden. When colleagues fail to show up, dependable staff members get called in on days off, work extended hours, or manage rushed handoffs. This pattern creates resentment and accelerates burnout among your best performers. Research shows that highly variable schedules increase caregiver turnover by up to 20%.
Looking to stabilize your caregiver workforce and reduce costly disruptions? Request a demo to see how HR Cloud's onboarding and engagement solutions help home care agencies build more reliable teams.
Beyond the immediate costs, chronic no-show problems create a vicious cycle. Scrambling to fill gaps leaves less time for thorough hiring and training. Rushed onboarding produces caregivers who feel unprepared and disconnected — making them more likely to become the next round of no-shows. Breaking this cycle requires addressing the root causes systematically.
|
Impact Category |
Cost/Consequence |
Timeline |
|
Administrative Time |
1-2 hours at $20-30/hour per incident |
Immediate |
|
Emergency Coverage |
20-30% premium pay above standard rates |
Same day |
|
Client Service Recovery |
Potential service refunds, relationship repair efforts |
1-7 days |
|
Reliable Staff Burnout |
Increased turnover risk (up to 20% higher) |
30-90 days |
|
Replacement Costs |
$2,600 per caregiver when turnover occurs |
60-90 days |
|
Client Churn |
Lost revenue from dissatisfied clients switching agencies |
30-180 days |
Why Caregivers Don't Show Up
Understanding why caregivers miss shifts is the first step toward prevention. While some no-shows result from genuine emergencies, most stem from fixable problems in how agencies hire, onboard, and manage their workforce.
|
Root Cause |
Warning Signs |
Prevention Strategy |
|
Rushed Onboarding |
High 90-day turnover (80%), frequent questions during shifts |
8+ hours orientation, 12+ hours ongoing training, chained task workflows |
|
Lack of Recognition |
Low engagement scores, minimal peer interaction |
Digital kudos platform, points-based rewards, public acknowledgment |
|
Inflexible Scheduling |
Frequent last-minute call-outs, high weekend no-show rates |
Preference tracking, advance notice for changes, shift-swap options |
|
Poor Communication |
Confusion about schedule changes, wrong client addresses |
Mobile app notifications, centralized messaging, read receipts |
|
Low Compensation |
Caregivers working multiple jobs, financial stress discussions |
Competitive wages, performance bonuses, earned wage access programs |
|
Isolation |
Caregivers report feeling disconnected, rarely attend meetings |
Team channels, regular check-ins, mentorship programs |
Rushed or Inadequate Onboarding
Agencies facing perpetual staffing shortages often prioritize speed over thoroughness in hiring. New caregivers get minimal orientation before being assigned to client homes. They don't understand expectations, lack confidence in their skills, and feel no connection to the organization. The 90-day turnover rate for home care sits around 80%, suggesting that many caregivers decide early on that the job isn't what they expected.
When onboarding consists of basic paperwork and a quick introduction, new hires lack the foundation to succeed. They're more likely to call out when facing challenging situations or simply disappear when better opportunities appear.
Lack of Connection and Recognition
Home care work can feel isolating compared to facility-based healthcare roles. Caregivers spend their days in client homes, rarely interacting with colleagues or supervisors. When they do excellent work, nobody notices. When they face challenges, they solve them alone. Over time, this isolation erodes organizational commitment and professional identity.
Employee engagement research consistently shows that recognition significantly impacts retention and attendance patterns. Yet home care agencies struggle to implement recognition systems that reach distributed workforces. Traditional employee appreciation programs designed for office environments don't translate well to caregivers who never visit headquarters.
Caregivers who feel like interchangeable labor rather than valued team members have little incentive to protect their attendance record. Why rearrange personal plans for an employer who doesn't acknowledge contributions or notice when you consistently show up? The transactional nature of many caregiver relationships — show up, complete tasks, get paid, repeat — creates minimal loyalty when competing demands arise.
Scheduling Challenges and Communication Gaps
Inflexible schedules that ignore caregiver preferences create attendance problems. When caregivers can't manage legitimate conflicts — doctor appointments, childcare issues, family obligations — they're more likely to call out or simply not show up rather than fight through rigid systems.
Communication breakdowns compound these issues. Changes made through phone tag, text messages, or paper schedules create opportunities for misunderstanding. A caregiver might genuinely believe their shift starts at 2 PM when the schedule shows 1 PM. Or they might never receive the message about a client address change.
Low Wages Without Compensating Benefits
The median hourly wage for home care aides remains stuck at $15.14 — far below the national living wage threshold. Fewer than 20% of caregivers receive employer-sponsored health insurance. When agencies can't compete on pay, they need to offer something else that makes caregivers prioritize their shifts.
Caregivers working multiple jobs naturally prioritize the better-paying position when scheduling conflicts arise. Without a strong workplace culture, growth opportunities, or meaningful recognition, your agency's shifts become expendable.
How Structured Onboarding Reduces No-Shows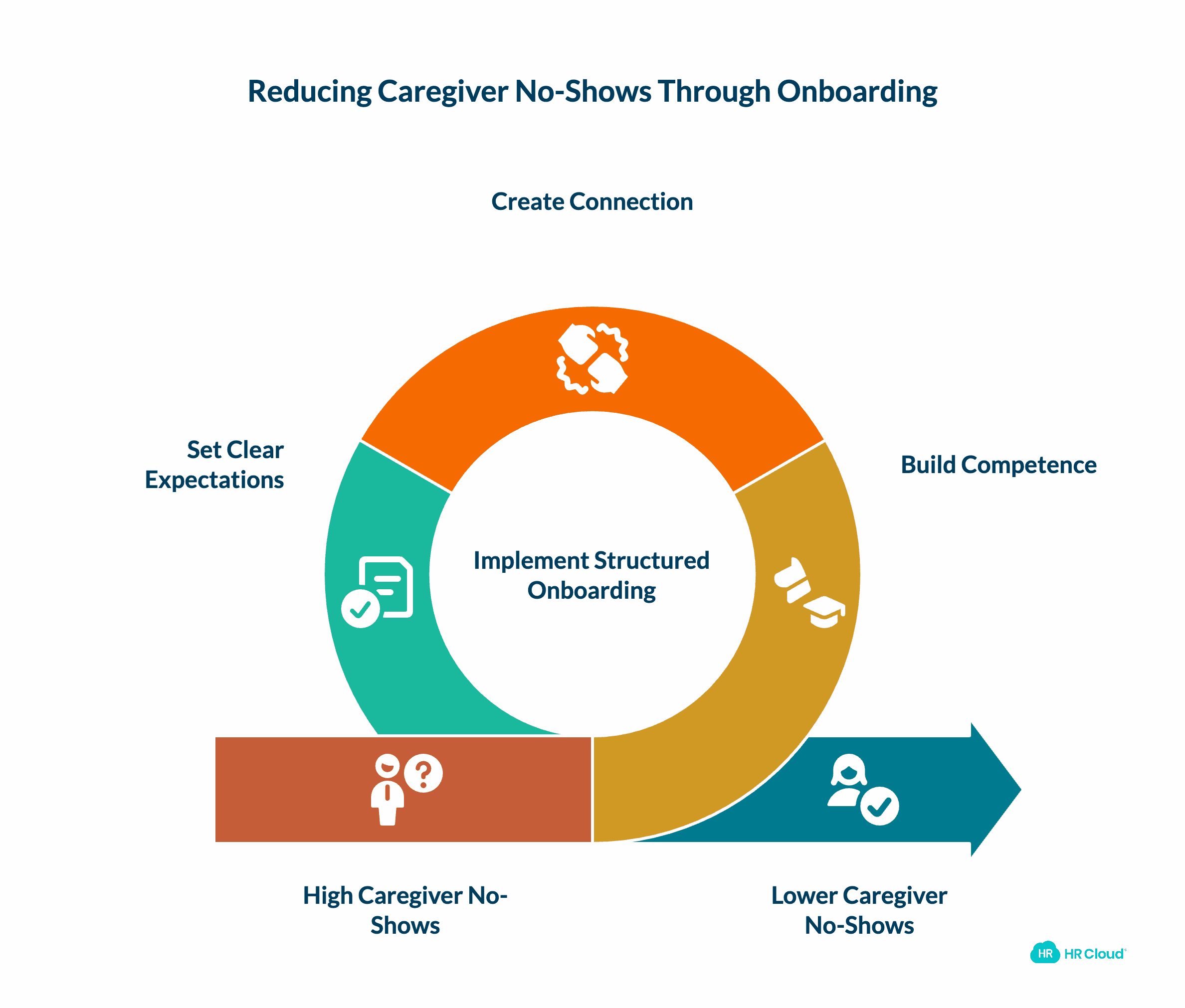
The foundation for reliable attendance starts on day one. Organizations with comprehensive onboarding programs see measurably lower early attrition, which directly correlates with better long-term attendance patterns.
Effective onboarding does more than process paperwork. It builds competence, connection, and commitment. New caregivers need to understand their role, feel prepared for challenges they'll encounter, and see a path forward within the organization.
Building Competence Through Training
Caregivers who receive at least eight hours of orientation and 12 hours of ongoing training show better job performance and higher retention. Agencies offering this level of training saw revenue increases averaging $346,000 — partially because they weren't constantly backfilling positions and could maintain fuller schedules.
Training builds confidence. Caregivers who've practiced difficult conversations, learned proper body mechanics for patient transfers, and understand emergency protocols feel equipped to handle their shifts independently. They're less likely to panic and call out when facing challenging situations.
Automated onboarding platforms deliver consistent training even when hiring multiple caregivers across different locations. Systems with customizable checklists can assign role-specific training modules, track completion, and trigger tasks based on hire date or employment status. Every new hire receives the same foundation regardless of which manager brings them on.
Chained task workflows ensure caregivers complete prerequisites before moving to advanced training. A caregiver can't access client-specific procedures until they've completed basic safety training. This sequencing prevents overwhelmed new hires from facing situations they're unprepared for — a common trigger for early call-outs.
Creating Connection Through Structured Check-ins
The first 90 days determine whether caregivers stay or leave. During this critical window, regular check-ins help new hires feel supported rather than abandoned.
Automated task management systems schedule check-in points at 7 days, 30 days, 60 days, and 90 days. Onboarding checklists trigger these touchpoints based on hire date, automatically assigning check-in tasks to managers with due dates and email reminders. These touchpoints give new caregivers opportunities to ask questions, share concerns, and receive feedback before small problems become reasons to quit.
Managers get visibility into which new hires might be struggling before those caregivers simply stop showing up. Task tracking shows which check-ins remain incomplete, alerting supervisors when managers aren't following through on scheduled conversations.
Mentorship programs amplify this effect. Pairing new caregivers with experienced colleagues provides ongoing support beyond formal check-ins. Mentors answer practical questions, provide encouragement, and help new hires navigate the social dynamics of the organization. Agencies with mentorship programs report lower overall turnover and fewer attendance issues.
HR Cloud’s onboarding tools support customizable checklists, forms, and workflow automation that help agencies standardize new-hire processes, assign onboarding tasks, and keep progress visible across the team. See how it works.
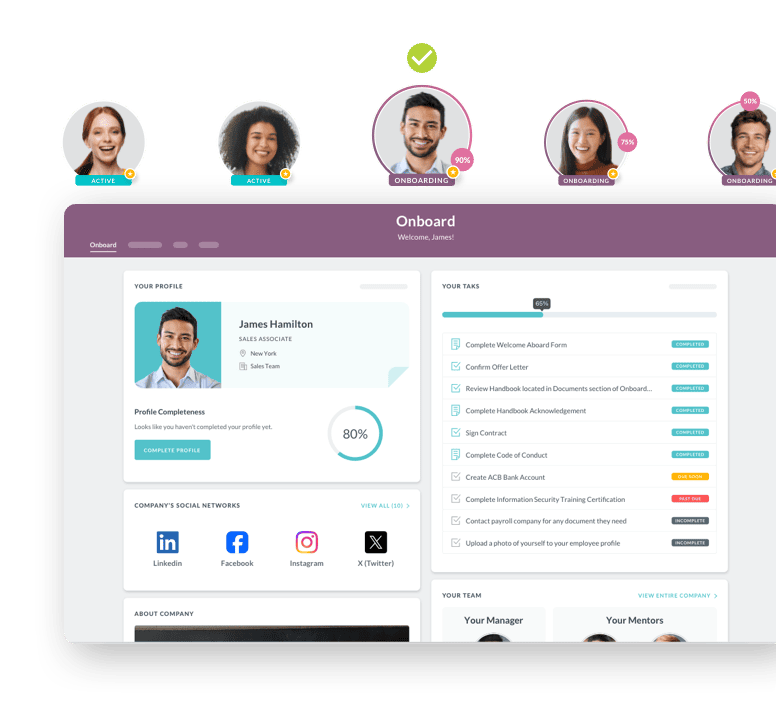
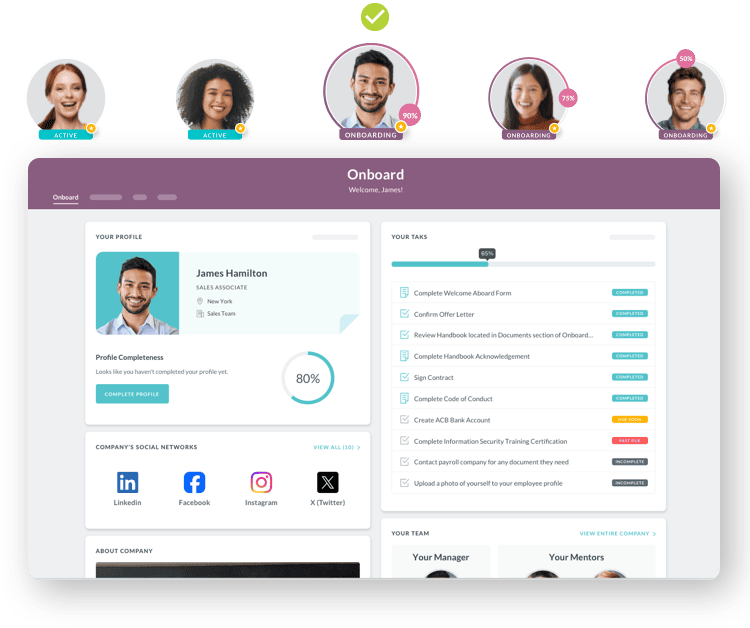
Setting Clear Expectations From the Start
Attendance policies work best when communicated clearly during onboarding. New caregivers should understand exactly how to report absences, what constitutes acceptable reasons for calling out, and what happens when attendance becomes problematic.
Digital onboarding platforms can require new hires to review and acknowledge attendance policies, emergency contact procedures, and shift confirmation processes. This creates documentation while ensuring caregivers can't claim they didn't know the rules.
|
Onboarding Component |
Ineffective Approach |
Effective Approach |
|
Training Duration |
2-4 hours, paperwork-focused |
8+ hours orientation, 12+ hours ongoing training |
|
Task Assignment |
Manual, inconsistent across managers |
Automated checklists triggered by hire date |
|
Check-in Schedule |
Ad hoc or when problems arise |
Structured at 7, 30, 60, 90 days |
|
Skill Verification |
Assume competence after orientation |
Chained tasks require prerequisite completion |
|
Policy Communication |
Verbal overview during first day |
Digital acknowledgment with documentation |
|
Mentorship |
Informal or nonexistent |
Structured pairing with experienced caregivers |
|
Manager Visibility |
Rely on caregiver self-reporting issues |
Automated tracking shows incomplete tasks |
Recognition and Engagement Strategies
Once caregivers complete onboarding, maintaining engagement becomes the next challenge. Recognition programs prove particularly effective in home care settings where caregivers work in isolation.
Making Invisible Work Visible
Caregivers doing excellent work in client homes receive no immediate validation. Office staff don't see the extra time they spend calming an anxious client or the creative problem-solving they use to accommodate a client's preferences. Recognition systems that surface these contributions make caregivers feel valued.
Digital recognition platforms let managers, colleagues, and office staff give kudos for specific achievements. A caregiver who handles a difficult client transition smoothly or covers a last-minute shift receives immediate, public recognition. When caregivers know their reliability gets recognized and appreciated, they're more likely to protect their track record.
Rewards That Reinforce Reliability
Pairing recognition with tangible rewards strengthens the impact. Points-based systems let caregivers accumulate recognition into rewards they value — gift cards, extra paid time off, or custom perks.
Agencies can design reward criteria specifically around attendance. Caregivers who complete a month with perfect attendance earn bonus points. Those who volunteer for hard-to-fill shifts get extra recognition. Creating a leaderboard around reliability gamifies attendance without feeling punitive.
The key is making rewards meaningful. Fifty cents worth of points feels insulting. Enough points for a $25 gift card or a movie night for the family feels valuable. Survey your caregivers to understand what rewards would actually motivate them.
|
Recognition Approach |
Impact on Attendance |
Implementation Complexity |
|
Verbal Praise Only |
Minimal - lacks tangibility |
Low |
|
Public Kudos (Digital Platform) |
Moderate - creates social accountability |
Medium |
|
Points Without Rewards |
Low - feels like empty gesture |
Medium |
|
Points + Gift Cards |
High - tangible value for reliability |
Medium |
|
Points + Custom Rewards |
High - personalized to caregiver preferences |
High |
|
Attendance Leaderboards |
Moderate - works for competitive personalities |
Low |
|
Perfect Attendance Bonuses |
High - directly incentivizes behavior |
Medium |
|
Peer Transfer Points |
Moderate - builds team culture |
Medium |
HR Cloud’s Workmates platform supports peer recognition through Kudos, including badges, points, and reward options such as gift cards and custom rewards, giving agencies a practical way to combine public appreciation with tangible incentives.
Building Community Through Communication Channels
Breaking through caregiver isolation requires intentional community-building strategies adapted for distributed workforces. When caregivers feel connected to colleagues and the organization, they're more invested in showing up and maintaining their professional reputation.
Internal communication platforms designed for distributed teams help agencies create virtual community spaces. Channels organized by location enable caregivers serving the same geographic area to connect and potentially cover each other's shifts. Specialty channels let caregivers working with dementia patients or hospice clients share specialized knowledge and emotional support. Interest-based channels build connections around topics unrelated to work, creating fuller relationships that strengthen organizational bonds.
Managers can use these channels strategically to maintain organizational culture even when staff never gather physically. Share wins publicly — a caregiver who received exceptional client feedback, someone who covered a difficult last-minute shift, or a team member who reached a service anniversary. These stories create shared narrative and reinforce what the organization values.
Chat functionality enables quick problem-solving that reduces the anxiety contributing to call-outs. A caregiver facing an unfamiliar medical situation can get immediate advice from a colleague who's handled something similar. Someone running late due to traffic can alert their relief caregiver directly rather than hoping the message reaches them through office staff. This real-time communication reduces the gaps where small problems escalate into no-shows.
Virtual team meetings via video platforms give caregivers rare opportunities to see colleagues and feel part of something larger than their individual client relationships. Monthly all-hands meetings, quarterly training sessions, or weekly huddles for specific teams create rhythm and belonging. Agencies report that caregivers who attend team meetings regularly show significantly better attendance patterns in their direct client care work.
Optimizing Scheduling to Prevent No-Shows
Even engaged, well-trained caregivers struggle with poor scheduling systems. Investing in better scheduling processes pays off through improved attendance.
Respecting Caregiver Preferences
Research consistently shows that caregivers who have some control over their schedules stay longer and show up more reliably. Agencies don't need to let caregivers write their own schedules, but incorporating preferences where possible makes a measurable difference.
Modern scheduling systems can capture caregiver preferences — preferred shift times, maximum weekly hours, days they need off, geographic boundaries for travel. Schedulers can then build schedules that accommodate these preferences while meeting client needs.
When schedule changes become necessary, giving caregivers advance notice and involving them in finding solutions shows respect. Scheduling platforms with mobile access let caregivers see their schedules anytime, request changes, and receive immediate confirmation. This transparency reduces misunderstandings that lead to missed shifts.
Leveraging Technology for Flexibility
Automated scheduling systems help agencies balance efficiency with flexibility. Intelligent algorithms can match caregiver availability and preferences with client needs, identify potential conflicts before they become problems, and suggest optimal coverage patterns.
Mobile apps give caregivers real-time access to their schedules. They can clock in and out from client homes with geolocation verification, confirm upcoming shifts, and request time off without playing phone tag with office staff. Push notifications remind caregivers about upcoming shifts and alert them to any changes.
Time Clock systems with geolocation restrictions ensure caregivers clock in from actual client locations rather than from home or in transit. This accountability reduces the ambiguity around shift start times that sometimes contributes to late arrivals or no-shows. When caregivers know their attendance is tracked accurately and automatically, they're more likely to maintain reliable patterns.
Time data can be exported or integrated with payroll systems, reducing manual processing. Accurate, timely payment improves caregiver satisfaction and reduces the financial stress that contributes to attendance problems.
|
Scheduling System Feature |
Manual/Paper-Based |
Spreadsheet-Based |
Automated Platform |
|
Caregiver Preference Tracking |
Lost sticky notes |
Static columns, rarely updated |
Dynamic profiles, easily updated |
|
Schedule Visibility |
Posted in office or texted |
Emailed files, version confusion |
Mobile app, real-time access |
|
Shift Confirmations |
Phone calls, no tracking |
Email trails, manual follow-up |
Automated reminders + confirmation |
|
Last-Minute Changes |
Multiple phone calls |
Mass email + hope |
Push notifications to available caregivers |
|
Conflict Detection |
Discovered when caregiver calls |
Requires manual checking |
Automatic alerts before assignment |
|
Time Tracking |
Paper timesheets, manual entry |
Digital forms, still manual entry |
Geolocation clock-in with export or integration options for payroll processing. |
|
Coverage Gaps |
Discovered too late |
Weekly review meetings |
Real-time dashboard alerts |
|
Reporting |
Manual tallies |
Basic formulas |
Automated analytics, trend identification |
HR Cloud’s Time Clock supports digital time tracking and can apply geolocation restrictions to clock-ins, helping agencies improve attendance accuracy and reduce manual time-entry work. Explore workforce management solutions for distributed home care teams.
Creating Accountability Through Visibility
When everyone can see the schedule, accountability improves. Caregivers who know their colleagues are counting on them to show up for their shift feel more responsibility than those working in isolation.
Shared visibility also helps identify patterns. Managers can quickly spot caregivers who frequently call out, consistently arrive late, or show other warning signs before those patterns escalate to no-shows. Early interventions — a conversation about what's causing the problems, offer of support or schedule adjustments — can prevent caregivers from reaching the point where they simply stop showing up.
Real-Time Communication Tools
The final piece of reducing no-shows involves upgrading how agencies communicate with caregivers. Outdated communication methods create the confusion that leads to missed shifts.
Moving Beyond Phone Tag
Agencies that still rely on phone calls and voicemails to communicate with caregivers face constant challenges. Messages get missed. Information gets garbled through successive retellings. Caregivers working shifts can't always answer their phones.
Text messaging improves on phone calls but creates its own problems. Important information gets lost in crowded message threads. There's no easy way to confirm who received which information. Personal phone numbers get mixed with work communication.
Internal messaging platforms solve these problems. All work communication happens in one place. Managers can send messages to individual caregivers, teams, or the entire organization. Read receipts show who received information. Searchable message history means caregivers can always find details about policy changes or special client instructions.
|
Communication Method |
Message Delivery |
Confirmation |
Information Retrieval |
Professional Boundaries |
|
Phone Calls |
Real-time but often missed |
Verbal only, no record |
Reliant on memory |
Personal phone usage |
|
Voicemail |
Delayed, often ignored |
None |
Must replay entire message |
Personal phone usage |
|
Text Messages (SMS) |
Fast but can be missed |
None (read receipts unreliable) |
Scroll through threads |
Personal phone usage |
|
|
Delayed, low open rates |
Sometimes (read receipts) |
Search possible but clunky |
Better but still personal |
|
Internal Platform |
Real-time with notifications |
Read receipts standard |
Full search, organized channels |
Separate work/personal |
Emergency Communication Protocols
Even with great systems, emergencies happen. Caregivers get sick, have car trouble, or face family crises that prevent them from working their shift. The difference between a manageable disruption and a client care disaster lies in how quickly the agency learns about the problem.
Clear protocols for reporting absences reduce chaos. Caregivers should know exactly how to report an absence (call a specific number, send a message to a designated person, use an app function), how much advance notice is expected, and what information to provide (reason for absence, whether they'll be available tomorrow, whether they know someone who could cover).
Digital systems can streamline this process. A caregiver calls out through an app. The system immediately alerts scheduling staff and begins presenting coverage options based on availability of backup caregivers. Office staff can respond to the emergency without needing to track down who was scheduled, where they were supposed to be, and who might be able to cover.
Client Communication Coordination
No-shows impact clients most directly. Strong communication systems help agencies manage client expectations and maintain trust even when caregiver attendance creates problems.
When a no-show occurs, clients should receive prompt communication about what's happening and when to expect a replacement caregiver. Automated systems can trigger client notifications when schedule changes occur, providing transparency that maintains trust.
Portal systems give clients visibility into their care schedule. They can see which caregiver is assigned to each shift, view caregiver profiles, and receive alerts about any changes. This reduces anxiety for clients who worry about unexpected visitors and helps them plan their days around care schedules.
Measuring and Improving
Reducing no-shows requires ongoing attention. Agencies need systems to track problems, identify patterns, and measure whether interventions work.
Tracking the Right Metrics
Start by establishing baseline metrics. What's your current no-show rate? Calculate this by tracking scheduled shifts versus completed shifts over a set period. Break this down by individual caregiver, shift type, and geographic area to identify patterns.
Track related metrics that provide context:
-
Time between hire and first no-show
-
Percentage of no-shows in first 90 days versus after
-
Day of week patterns (do no-shows spike on Fridays or Mondays?)
-
Caregiver characteristics (full-time versus part-time, years of experience)
Modern workforce management platforms can generate these reports automatically, highlighting trends that might not be visible when looking at individual incidents.
|
Metric |
Calculation |
Target Benchmark |
What It Reveals |
|
Overall No-Show Rate |
(Missed shifts ÷ Scheduled shifts) × 100 |
<5% |
Overall workforce reliability |
|
New Hire No-Show Rate |
No-shows in first 90 days ÷ Total new hire shifts |
<8% |
Onboarding effectiveness |
|
Repeat Offender Rate |
Caregivers with 3+ no-shows ÷ Total workforce |
<3% |
Need for performance management |
|
Friday/Monday Spike |
Weekend border no-shows ÷ Average daily no-shows |
<1.5x |
Scheduling or burnout issues |
|
Last-Minute Call-Out Rate |
Call-outs <4 hours before shift ÷ Total no-shows |
<30% |
Communication/engagement problems |
|
Coverage Success Rate |
Gaps filled ÷ Total no-shows |
>90% |
Backup system effectiveness |
|
Cost Per No-Show |
(Admin time + Premium pay + Service recovery) ÷ No-shows |
Track trend |
Financial impact visibility |
Using Data to Target Interventions
Once you understand your patterns, target interventions strategically. If most no-shows occur in the first 90 days, focus on improving onboarding and early check-ins. If certain shifts have higher no-show rates, investigate whether those shifts have scheduling issues, difficult clients, or other factors that make them less desirable.
Test interventions systematically. Implement a new approach with one group of caregivers while maintaining current practices with a control group. Measure results over several months before deciding whether to roll out changes organization-wide.
Building Accountability Without Punishment
Nobody performs well under purely punitive systems. While attendance problems need consequences, effective accountability systems focus on understanding and solving problems rather than simply disciplining caregivers.
When caregivers have attendance issues, start with conversation. What's causing the problem? Do they face scheduling conflicts, transportation challenges, or issues with specific clients? Can the agency help address underlying problems?
Document attendance concerns through performance management systems that track conversations and create specific performance goals with measurable targets. Goal tracking features let managers set attendance targets (e.g., "Achieve 95% shift completion rate over next 30 days") and monitor progress through regular check-ins. This structured approach gives caregivers clear expectations and visible accountability.
Performance review cycles can incorporate attendance metrics alongside quality measures, creating balanced evaluations that recognize reliable caregivers while addressing problems directly. When caregivers see that attendance matters in their formal reviews and affects their standing, they take it more seriously.
Reserve disciplinary action for caregivers who refuse to improve despite support and clear expectations. For those situations, having documented conversations, performance goals with tracked progress, and attendance policies makes difficult decisions clearer and more defensible.
HR Cloud’s Perform tools support goal tracking, progress check-ins, and performance reviews, giving agencies a more structured way to monitor expectations and discuss performance over time
Implementation Timeline: From Assessment to Results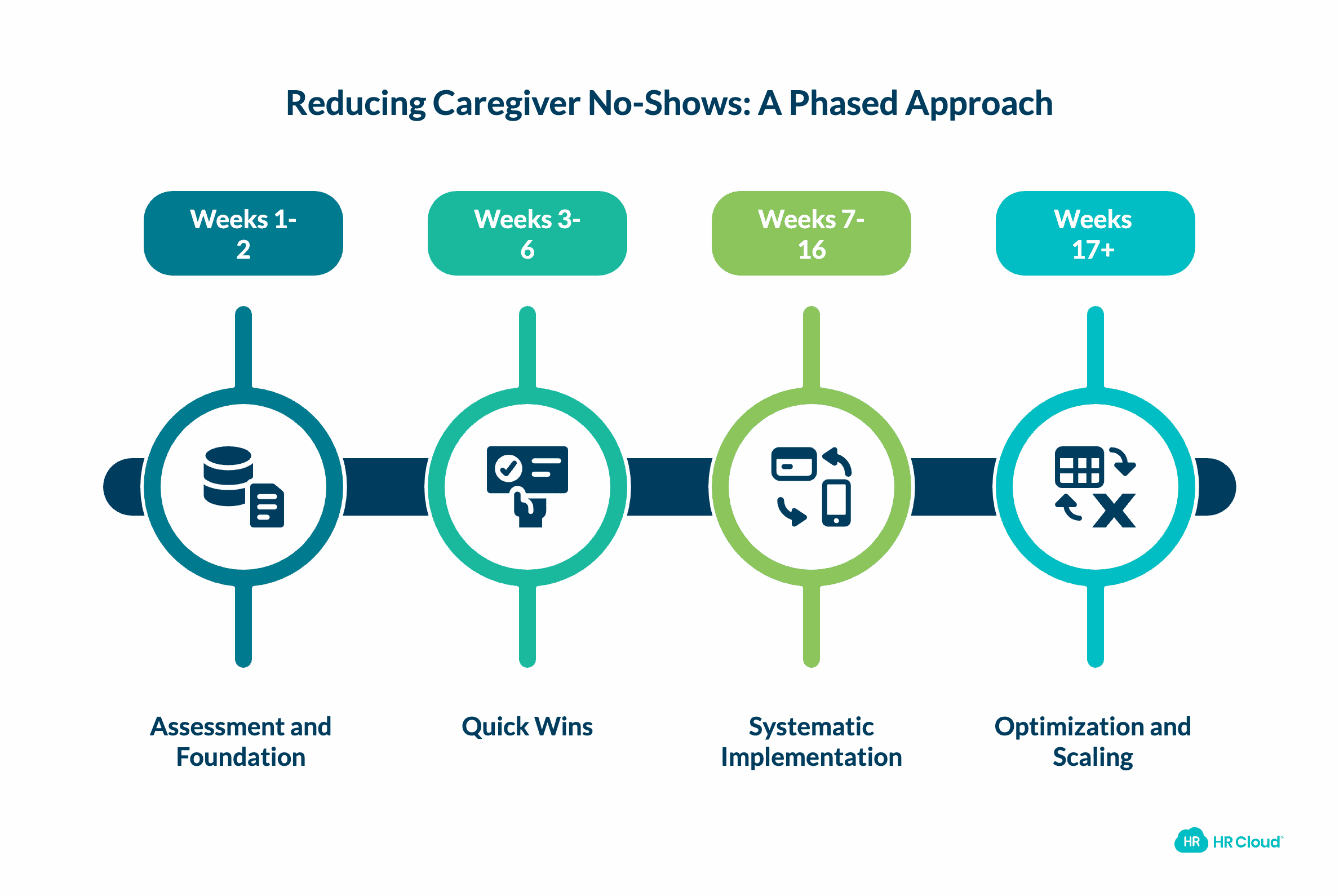
Reducing caregiver no-shows requires a phased approach that builds momentum through quick wins while establishing sustainable systems for long-term improvement.
Phase 1: Assessment and Foundation (Weeks 1-2)
Start by understanding your current state. Calculate your baseline no-show rate across different dimensions: overall agency, by shift type, by caregiver tenure, and by day of week. This data reveals patterns that guide your intervention strategy.
Survey caregivers anonymously about why they miss shifts. The answers often surprise managers. Transportation challenges, childcare conflicts, and communication confusion rank higher than most agencies expect. Understanding actual causes beats assumptions every time.
Review your current onboarding process honestly. Time how long orientation actually takes. Document what new caregivers learn versus what they need to know. Identify gaps between policy documents and reality.
This assessment phase requires minimal budget but delivers critical insights. Agencies that skip this step often implement solutions that address the wrong problems.
Phase 2: Quick Wins (Weeks 3-6)
Target interventions that show fast results and build organizational confidence in the improvement process.
Implement digital shift confirmations. Before every shift, caregivers receive an automated reminder asking them to confirm they'll be there. This simple step reduces genuine misunderstandings about schedule details and creates accountability. Agencies report 15-25% reduction in no-shows from confirmation systems alone.
Launch a perfect attendance recognition program. Caregivers who complete a month with zero no-shows receive public acknowledgment and small rewards. The visibility creates social proof that reliability matters and gets noticed.
Streamline the call-out process. Give caregivers one clear number to call and one backup digital option. Confusion about how to report absences causes some no-shows — caregivers try to reach the wrong person, can't get through, and give up.
These quick wins generate results within weeks, creating momentum for larger changes.
Phase 3: Systematic Implementation (Weeks 7-16)
Roll out comprehensive solutions that address root causes systematically.
Redesign onboarding to include structured check-ins at 7, 30, 60, and 90 days. Automated systems trigger these conversations regardless of manager workload. The consistency helps new caregivers feel supported during the vulnerable early months when most turnover occurs.
Deploy mobile scheduling access for all caregivers. Real-time visibility into their schedules, ability to request changes through approved workflows, and push notifications about updates reduce the scheduling confusion that contributes to missed shifts.
Build internal communication channels that break through isolation. Caregivers working alone in client homes need connection to the broader team. Digital platforms enable sharing challenges, asking questions, and receiving support even when physically separated.
This phase requires more investment but creates the infrastructure for sustained improvement.
Phase 4: Optimization and Scaling (Weeks 17+)
Refine approaches based on data and expand successful interventions.
Analyze which recognition types drive the most attendance improvement. Some caregivers value gift cards; others prefer extra paid time off or professional development opportunities. Customize rewards to maximize impact.
Track which onboarding components correlate with better long-term attendance. Agencies often discover that specific training modules or mentor pairings predict caregiver reliability. Double down on what works.
Use scheduling data to identify patterns invisible to manual tracking. Maybe Tuesday evening shifts have higher no-show rates. Or perhaps caregivers assigned to clients more than 30 minutes from home call out more frequently. Data reveals optimization opportunities.
The improvement process never fully completes. Workforce dynamics evolve, client needs shift, and labor market conditions change. Agencies that treat attendance optimization as ongoing rather than one-time projects maintain competitive advantages.
|
Implementation Phase |
Key Actions |
Expected Impact |
Timeline |
|
Assessment |
Calculate baselines, survey caregivers, audit onboarding |
Understanding root causes |
Weeks 1-2 |
|
Quick Wins |
Shift confirmations, recognition launch, simplified call-outs |
15-25% no-show reduction |
Weeks 3-6 |
|
Systematic |
Automated check-ins, mobile scheduling, team communication |
30-40% no-show reduction |
Weeks 7-16 |
|
Optimization |
Data analysis, customized rewards, pattern identification |
50%+ no-show reduction |
Weeks 17+ |
Creating a Culture of Reliability
Reducing no-shows isn't about implementing individual tactics. It's about building a culture where showing up matters and where caregivers want to protect their reputation for reliability.
Agencies with the lowest no-show rates share common characteristics. They hire deliberately, prioritizing cultural fit alongside skills. They invest in thorough onboarding that builds competence and connection through automated workflows that deliver consistent experiences. They communicate clearly through internal channels that break through isolation. They recognize and reward reliability through public acknowledgment and tangible incentives while addressing problems directly through documented performance management.
These agencies understand that caregivers make rational decisions about where to invest their time and energy. When showing up means joining a supportive team, doing meaningful work, receiving fair recognition, and having growth opportunities tracked through clear goals, caregivers choose to be reliable. When showing up means another isolating shift for an employer who doesn't notice or care, caregivers prioritize other commitments.
The home care industry faces legitimate workforce management challenges. With 59% of agencies reporting caregiver shortages and 75% turnover rates, competition for qualified staff will intensify. But agencies that treat no-shows as symptoms of fixable problems rather than inevitable costs gain competitive advantages. They build more stable teams through structured onboarding, deliver more consistent client care through better scheduling, and spend fewer resources on perpetual hiring because their retention improves.
The strategies outlined — from automated onboarding workflows to recognition programs to mobile scheduling access — work together synergistically. Implementing even one or two creates measurable improvement. Combining multiple approaches addresses no-shows from different angles, creating reinforcing effects that compound over time.
Start with assessment to understand your specific patterns, implement quick wins to build momentum, then systematically address root causes through technology and process improvements. The investment in better workforce management systems pays returns through reduced turnover costs, improved client satisfaction, and stronger competitive positioning in markets increasingly focused on care quality and consistency.
Ready to reduce caregiver no-shows and build a more reliable workforce? Request a demo to see how HR Cloud’s onboarding, recognition, and workforce management tools can help home care agencies support more consistent attendance, stronger communication, and better caregiver retention.
 Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Frequently Asked Questions
What's the average cost of a caregiver no-show?
Individual no-shows cost $150-250 per incident in direct expenses (administrative time, premium pay for replacements, client service recovery). However, chronic no-shows lead to full caregiver replacement at $2,600 per position. Agencies experiencing 5% no-show rates with 50 caregivers face approximately $65,000 in annual replacement costs attributable to attendance-related turnover.
How quickly should we address caregiver attendance problems?
Address attendance concerns after two unexcused absences or three late arrivals within 30 days. Early intervention often reveals solvable problems like transportation issues, scheduling conflicts, or personal challenges. Waiting until patterns become severe makes intervention less effective and creates documentation gaps if termination becomes necessary.
Can recognition programs really improve attendance?
Yes. Agencies prioritizing workplace culture and recognition saw caregiver turnover drop from 79% to 75% according to the 2025 Activated Insights report. Recognition programs work best when tied to specific behaviors like perfect attendance or covering difficult shifts, and paired with meaningful rewards caregivers actually value. The key is making recognition timely, specific, and visible to create social accountability.
What's more important for reducing no-shows — better pay or better culture?
Both matter sequentially. Pay must meet a competitive threshold first — if you're paying significantly below market rates ($15.14 median hourly wage), no amount of recognition will retain caregivers. Once pay reaches competitive levels, culture becomes the primary differentiator. The most effective approach combines fair compensation with strong culture built around recognition, communication, and growth opportunities.
How do we balance flexibility with accountability?
Separate legitimate needs from unreliability patterns. Build systems accommodating legitimate flexibility through shift swapping, advance time-off requests, and preferred schedule preferences. Maintain clear expectations about notification procedures and acceptable absence reasons. Consistent policy application prevents perceptions that certain caregivers receive special treatment. Document both accommodations offered and accountability measures taken.
Should we use automated scheduling systems?
Agencies with 15+ caregivers typically see ROI from scheduling automation within 3-6 months through reduced administrative time, fewer scheduling errors, and better optimization of caregiver-client matching. Smaller agencies might start with basic digital calendars and upgrade as they grow. Essential features include mobile caregiver access, geolocation time tracking, and payroll integration to eliminate duplicate data entry.
What role does onboarding play in preventing future no-shows?
Comprehensive onboarding proves critical for long-term attendance reliability. Agencies offering eight hours of orientation and 12 hours of ongoing training see significantly better retention and fewer early no-shows. Strong onboarding builds competence through skill development, creates connection through structured check-ins and mentorship, and sets clear expectations about attendance policies before problems develop. The 90-day period determines whether caregivers stay or leave.
How do we maintain accountability without creating a punitive environment?
Focus on understanding before punishing. When attendance issues arise, start with conversations exploring underlying causes rather than immediate discipline. Create specific performance goals offering support while setting clear expectations and measurable targets. Document everything for consistency and legal protection. Reserve disciplinary action for caregivers who won't improve despite support and clear communication. This approach addresses problems while maintaining a culture where people feel valued rather than constantly monitored.
What metrics indicate our attendance improvement strategies are working?
Track no-show rate trends over time, broken down by caregiver tenure (first 90 days vs. tenured staff), shift type, and day of week. Improving metrics include: overall no-show rate declining below 5%, new hire no-show rates dropping below 8%, repeat offenders (3+ no-shows) staying under 3% of workforce, and coverage success rates exceeding 90%. Additionally monitor related indicators like caregiver satisfaction scores, time-to-fill for emergency coverage, and client retention rates.
How long does it take to see measurable improvement in attendance?
Quick wins like digital shift confirmations and simplified call-out procedures show results within 3-6 weeks, typically reducing no-shows by 15-25%. Systematic interventions including redesigned onboarding and mobile scheduling deliver 30-40% improvement within 4-6 months. Full cultural transformation achieving 50%+ reduction requires 6-12 months of sustained effort across multiple initiatives. The key is starting with quick wins that build organizational confidence while implementing deeper systemic changes.

Keep Reading
How Long Does ADP Onboarding Take? (And How to Reduce It)
The short answer: administrative onboarding in ADP Workforce Now (WFN) takes 1–5 business
ADP Workforce Now Onboarding Checklist: What's Missing (and How to Fix It)
According to Gallup, only 12% of employees strongly agree their organization does a great
HR Software for Hospitals: What to Look for in 2026
Hospital HR teams in 2026 face a specific set of problems: chronic staffing shortages,
Like What You Hear?
We'd love to chat with you more about how HR Cloud® can support your business's HR needs. Book Your Free Demo

Build a Culture of Recognition. Boost Engagement. Guaranteed.
Workmates empowers employees to stay informed, connected, and appreciated—whether they’re on the front line, in the office, or remote. Recognition drives 12x higher engagement.Trusted by industry leaders in every sector




Cut Onboarding Costs by 60%.
Take the confusion and follow-ups out of onboarding with automated workflows, digital forms, and structured portals—so new hires ramp faster 3X quicker.Trusted by industry leaders in every sector