Healthcare Employee Engagement: The 2026 Strategic Guide for Hospitals, Clinics, and Senior Care

- Why Healthcare Employee Engagement Matters More in 2026
- The Unique Challenges of Healthcare Employee Engagement
- Healthcare Employee Engagement Strategies That Work
- Connecting Engagement to Compliance (Not Against It)
- Technology Enablement for Deskless Healthcare Workers
- Measuring Healthcare Employee Engagement
- How to Build Healthcare Employee Recognition Programs That Resonate?
- Segment-Specific Engagement Playbooks
- How HR Cloud Supports Healthcare Engagement at Scale
- The Only Engagement Strategy That Actually Sticks

 Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.
Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.

The conventional wisdom around employee engagement goes something like this: build a strong culture and the right people will come, and stay.
That's largely true for typical industries, but in healthcare, framing engagement purely as a culture conversation is a luxury the industry can no longer afford.
In 2024, hospital turnover hit 22.7%.
Nursing turnover sat at 27.1%.
And senior care CNAs were leaving at rates exceeding 40% in several markets.
These are financial emergencies hiding inside workforce reports because
Replace one registered nurse, and you've spent between $52,000 and $64,000.
Replace a physician, and you're looking at half a million and sometimes more.
When you multiply those figures by your annual turnover rate, you can see that engagement is one of the highest-leverage financial decisions your organization makes every year.
The organizations pulling ahead in the retention battle aren't necessarily spending more on engagement programs. They've built engagement into their operational infrastructure — as deliberately as they build clinical workflows — across onboarding, compliance, communication, and recognition.
And, more importantly, they've built it for the workforce they actually have: deskless, shift-based, emotionally invested, and spread across hospitals, outpatient clinics, and senior care facilities with very different needs.
This guide covers all of it. A practical, segment-specific set of healthcare employee engagement strategies, with a 90-day roadmap your team can start acting upon this month.
Why Healthcare Employee Engagement Matters More in 2026
The argument for employee engagement in healthcare has never been stronger or more urgent. But it's no longer just about retention statistics. In 2026, the stakes have expanded to
-
patient safety
-
reimbursement rates
-
long-term financial sustainability
The American Hospital Association reports that the healthcare industry will face a shortage of up to 124,000 physicians and more than 200,000 nurses by 2033. Meanwhile, Gallup research consistently shows that only 23% of employees globally feel engaged at work. And healthcare workers, carrying pandemic-era burnout that never fully resolved, are particularly vulnerable to disengagement.
Here's what that means in practice: Low engagement among healthcare employees bleeds directly into patient outcomes.
Research from Press Ganey has documented for years that organizations in the top quartile for staff engagement experience 41% fewer patient safety incidents.
The financial case is equally compelling. With registered nurse turnover costing hospitals between $52,350 and $64,000 per departure and physician turnover ranging from $500,000 to $1 million, the ROI of engagement isn't abstract. It's the difference between running lean and running on fumes.
Engaged healthcare organizations consistently use 30–40% less agency staffing, cutting some of the most expensive line items in their operational budgets.
And then there's what 2026 specifically brings.
Value-based care models now tie reimbursement directly to patient outcomes and satisfaction. The Gen Z clinical workforce entering hospitals, clinics, and care facilities in meaningful numbers expects transparency, communication, and purpose-driven work from day one.
The organizations that will thrive are those who stop treating healthcare employee satisfaction as a soft metric and start managing it with the same rigor as their financial performance.
The Unique Challenges of Healthcare Employee Engagement
|
Challenge |
Hospitals |
Outpatient Clinics |
Senior Care |
Home Health |
|
Deskless workforce access |
Very High |
Medium |
Very High |
Very High |
|
Multi-site culture inconsistency |
High |
High |
Medium |
Medium |
|
Compliance training burden |
Very High |
Medium |
High |
High |
|
Shift-based communication gaps |
High |
Medium |
High |
Very High |
|
Frontline staff turnover |
High |
Medium |
Very High |
Very High |
You know, if your engagement efforts haven't worked until now, it's probably because your engagement frameworks were built for office workers while your workforce operates in 12-hour shifts, split across multiple floors, facilities, and care settings. And that too often without reliable access to email or a desktop computer.
Healthcare is uniquely complex and that complexity shapes everything.
Let’s discuss some of those challenges.
Challenge #1. Clinical vs. Administrative Staff Needs
The divide between clinical and administrative staff in healthcare is wider than it looks on an org chart.
Clinical workers — nurses, CNAs, allied health professionals, surgical techs — are deskless by definition. They work alongside patients, not computers. They move constantly. They clock in and out of shifts spanning day, evening, and overnight hours.
Traditional engagement tools built around email newsletters, intranet portals, and desktop-first platforms fundamentally fail this group.
The nurse finishing a night shift doesn't have bandwidth to log into an HR portal to acknowledge a company announcement.
The CNA heading into a memory care unit can't check a desktop app for a compliance training reminder.
Designing your engagement strategy around administrative staff means leaving your frontline clinical workers — your highest-turnover population — hanging.
Challenge #2. Multi-Site Healthcare Management Complexity
For hospital systems, multi-clinic networks, or senior care chains, engagement complexity compounds with every additional site.
Every new facility brings its own culture, its own management dynamics, and its own operational realities. What works beautifully at your flagship hospital may land flat at a rural satellite clinic.
And technology fragmentation makes it worse.
When facilities run their own communication tools, recognition platforms, or HR systems, which may be different from others, you end up with inconsistent employee experiences and cultures.
The CNA at your downtown facility gets a peer recognition shoutout on a shared platform. Her counterpart at the assisted living facility across town gets nothing because their location never rolled out the program. These gaps, small as they seem, are definitely noticed.
Challenge #3. Engagement Fatigue due to Compliance Pressure
When the first message a new employee receives is a list of mandatory training modules due within 30 days, you've begun the relationship with a demand, not a welcome.
But this is also the compliance reality in healthcare. And I hear you.
The average hospital nurse completes between 30 and 60 hours of mandatory training annually, possibly more. And that's on top of a full patient care workload.
In senior care, where staffing ratios are already stretched, CNAs are expected to complete annual dementia care training, infection control certifications, abuse prevention modules, and CMS-mandated requirements, often on their own time.
But the volume isn't the only issue.
Most healthcare compliance training is delivered through systems that were not designed with the end user in mind. They consist of long desktop-based modules, dense regulatory language, and knowledge checks that test memorization rather than application.
The answer is not to cut compliance but to redesign how it is delivered and explained, which we will explore in the next section.
Healthcare Employee Engagement Strategies That Work
The strategies that actually work in healthcare employee engagement share one common characteristic: they are designed for the real operational context of clinical work, not borrowed from a generic HR playbook for largely desk-based employees.
Here's what that looks like in practice, broken down by care setting.
Hospital Employee Engagement Best Practices
Hospitals present the most complex engagement environment — large teams, multiple departments, 24/7 operations, and a culture where hierarchy has historically been rigid. The engagement levers that consistently move the needle are those that give clinical staff a voice and make their daily work meaningful.
Unit-based shared governance councils, where nurses actively participate in decisions about staffing, scheduling, and care protocols, are one of the most consistently effective approaches in acute care settings. They work because they address a root cause of disengagement: the feeling of having no say. When nurses help design their own work environment, ownership happens automatically.
Hospital nurse engagement strategies also need to account for the physician-nurse dynamic. Hospitals where physicians and nurses actively collaborate on quality improvement initiatives show measurably higher engagement scores for both groups. Interdisciplinary rounds, structured communication training, and shared accountability for patient outcomes all reinforce the sense that every role matters.
For a deeper dive into creating positive work environments and patient-centered care approaches, see HR Cloud's guide on how to increase employee engagement in healthcare.
Clinic Staff Engagement Approaches
Outpatient and ambulatory clinics have their own engagement dynamics. Smaller teams mean culture is more visible and more fragile simultaneously.
One disengaged physician or office manager can affect the entire team's morale in ways that wouldn't even register in a 500-bed hospital.
The most effective engagement levers in clinic settings center on provider-staff collaboration and shared ownership of patient experience. Clinics that hold brief end-of-week team huddles to celebrate patient outcome wins and discuss process improvements consistently report stronger team cohesion.
The wins need to be real and specific. For instance, "The MA caught the medication discrepancy that prevented a readmission. Kudos to that."
Flexible scheduling is another powerful engagement driver for medical staff engagement. In smaller clinical environments, some scheduling flexibility signals that the organization sees them as human beings, not schedule units. That matters more than you might think.
Senior Care Employee Engagement Tactics
Senior care presents the highest-stakes engagement challenge in healthcare.
CNA turnover in long-term care exceeds 40% in many markets, and the emotional demands of the work — particularly in memory care — create compassion fatigue that no engagement program alone can fully address.
The strongest senior-care engagement strategies are relational at their core. Programs that acknowledge the emotional load caregivers have to carry have a clear impact on engagement and retention. This can be done through peer support forums, consistent leader rounding, and recognition that values intent and involvement more than operational output.
Resident–staff connection programs, where CNAs and care aides build ongoing relationships with specific residents, reinforce the sense of purpose that brought many into caregiving. When recognition highlights those specific moments of connection, rather than only tenure, the effect becomes even stronger.
For quick-win tactics that work across all three settings, read this: 9 simple ways to improve employee engagement in healthcare.
Strategy #1. Building a Foundation: Onboarding + Engagement Integration
Here's something I've observed consistently in healthcare HR: organizations that treat onboarding and engagement as separate initiatives almost always struggle with both. And organizations that design them as a single, connected system tend to see dramatically better outcomes.
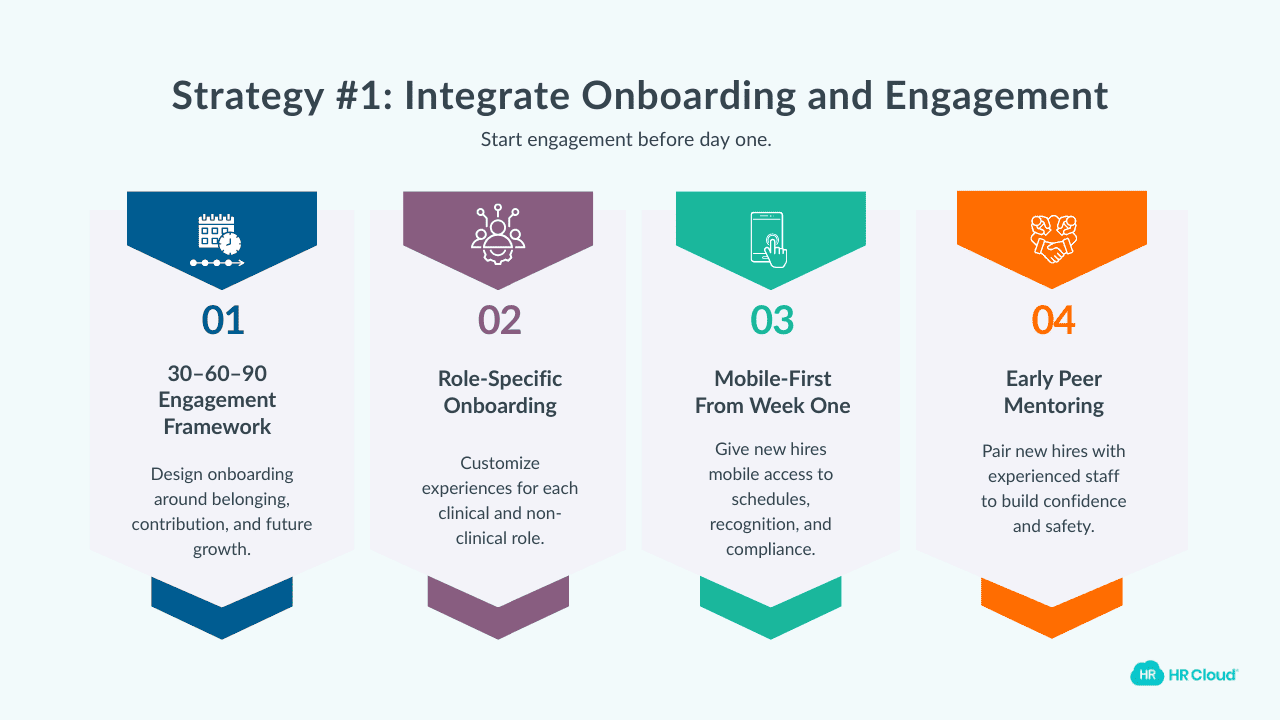
90-day Engagement Framework
Engagement doesn't begin after onboarding ends, or after Day 30, 60, or 90 of onboarding. It begins before day 1. That’s why engagement should be an integral part of the 30-60-90-day onboarding framework.
Here are a few things you can do to build that foundation:
The first 90 days matter enormously in healthcare because this is the highest-risk period for turnover and the highest-leverage window for connection.
-
At 30 days, the focus should be on belonging: Does this new employee know their colleagues, understand the unit's culture, and feel safe asking questions?
-
At 60 days, it should shift to contribution: Are they demonstrating the competencies that matter, and do they feel their work has an impact?
-
At 90 days, the question is trajectory: Do they see a future here?
Role-specific onboarding
This is non-negotiable because a hospital-wide, one-size-fits-all orientation is one of the most expensive mistakes in healthcare HR.
The experience for a new RN, a travel physician, an allied health tech, and an administrative specialist should feel fundamentally different because their roles, their risk exposure, and their day 1 realities are entirely different.
Personalising employee experiences in healthcare is a retention strategy and you should not skimp on that.
Mobile-first HR Tools
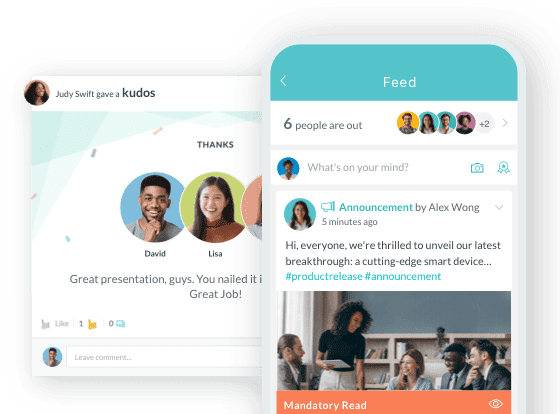
For deskless clinical workers especially, access to mobile-first recognition platforms, schedule management, and communication apps from the first week of employment sends a powerful signal. It communicates that your organization built systems for how they actually work.
A nurse who can access her schedule, submit a PTO request, and acknowledge a colleague's recognition post from her phone during a break can see that the organization is invested in them and hence be more open to engage.
Peer mentoring programs
Continued peer mentoring during onboarding is much better than formal orientation events for engagement.
A new CNA paired with a senior colleague who can answer real questions builds the psychological safety that supports better judgment and calmer decision-making. Questions such as:
-
Who do I actually call for help at 2 a.m.?
-
What do I do when a resident refuses care?
-
What should I do if I make a mistake, even a small one?
-
What should I document immediately, and what can wait?
-
How do I navigate family members who are upset or demanding?
- When is it appropriate to escalate to a nurse, and when should I try another approach first?
Make compliance training part of onboarding, not separate from it. When new hires complete required training in the same platform where they meet their team, compliance feels like part of the process, not an extra burden.


Connecting Engagement to Compliance (Not Against It)
Let's talk about something most engagement guides completely ignore: the relationship between mandatory compliance training and employee engagement. Because right now, in most healthcare organizations, those two things are working against each other.
The compliance-engagement paradox is real.
The Joint Commission, CMS, OSHA, and state licensing boards collectively require hundreds of hours of mandatory training from your clinical staff over the course of their employment.
When that training is delivered through outdated desktop-only systems in dense text formats, during already-exhausted shift transitions, it doesn't just create friction. It erodes the willingness to work.
The organizations getting this right have made a few key shifts.
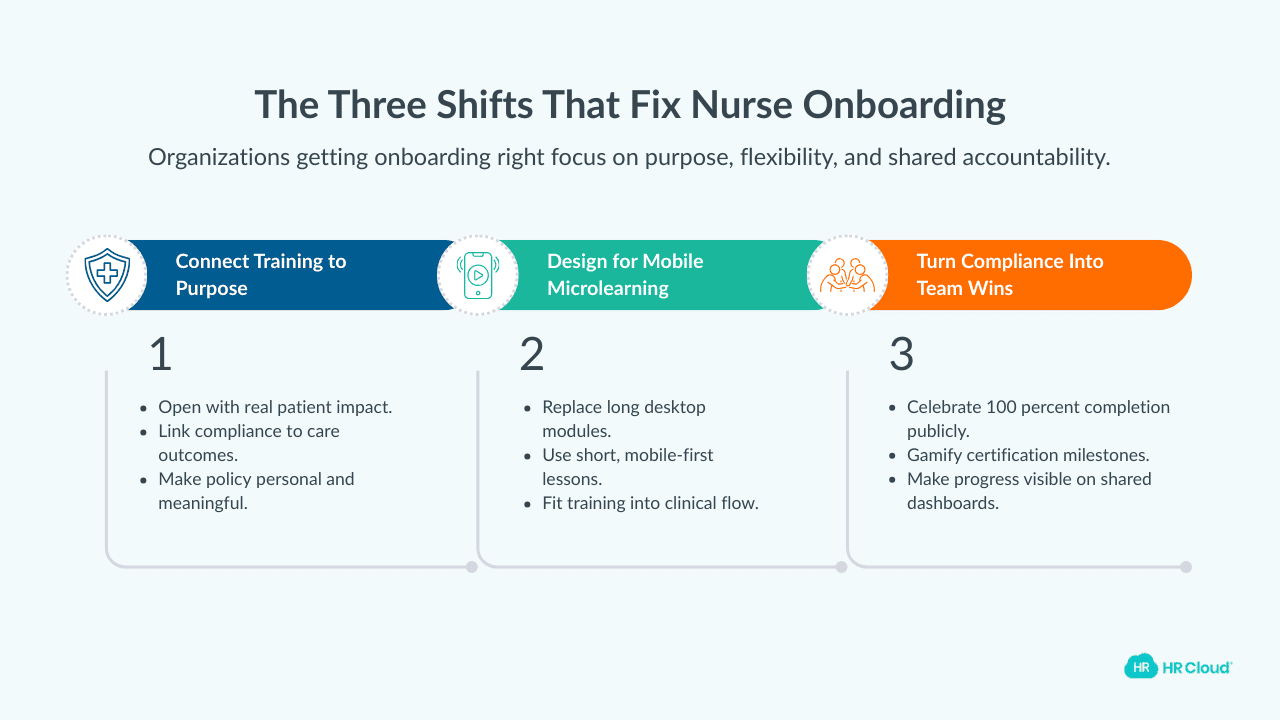

First: connect training to purpose, not just policy
When HIPAA training opens with a real patient story about what went wrong when information was shared without consent — and how it affected the patient — staff engage differently than when it opens with a regulatory citation. Purpose-connected learning improves both completion rates and retention.
Second: use mobile-first, microlearning formats
A 45-minute desktop training module is a credentialing system designed for an era when clinical staff had time to sit at computers. A 7-minute mobile module with a short knowledge check — completable during a break or between patient rooms — actually gets done. And it actually gets remembered.
Third: celebrate compliance milestones as the team wins
When a unit completes 100% of their annual training, acknowledge it publicly. Gamify the certification process through your recognition platform. Make progress visible on shared team dashboards. These small shifts reframe compliance from individual burden to collective achievement.
Technology Enablement for Deskless Healthcare Workers
70-80% percent of the global workforce is deskless. In healthcare, that number is closer to 90%. And yet the majority of HR technology — including most engagement platforms — was designed for the 10%. This gap is one of the defining engagement problems in healthcare HR today.
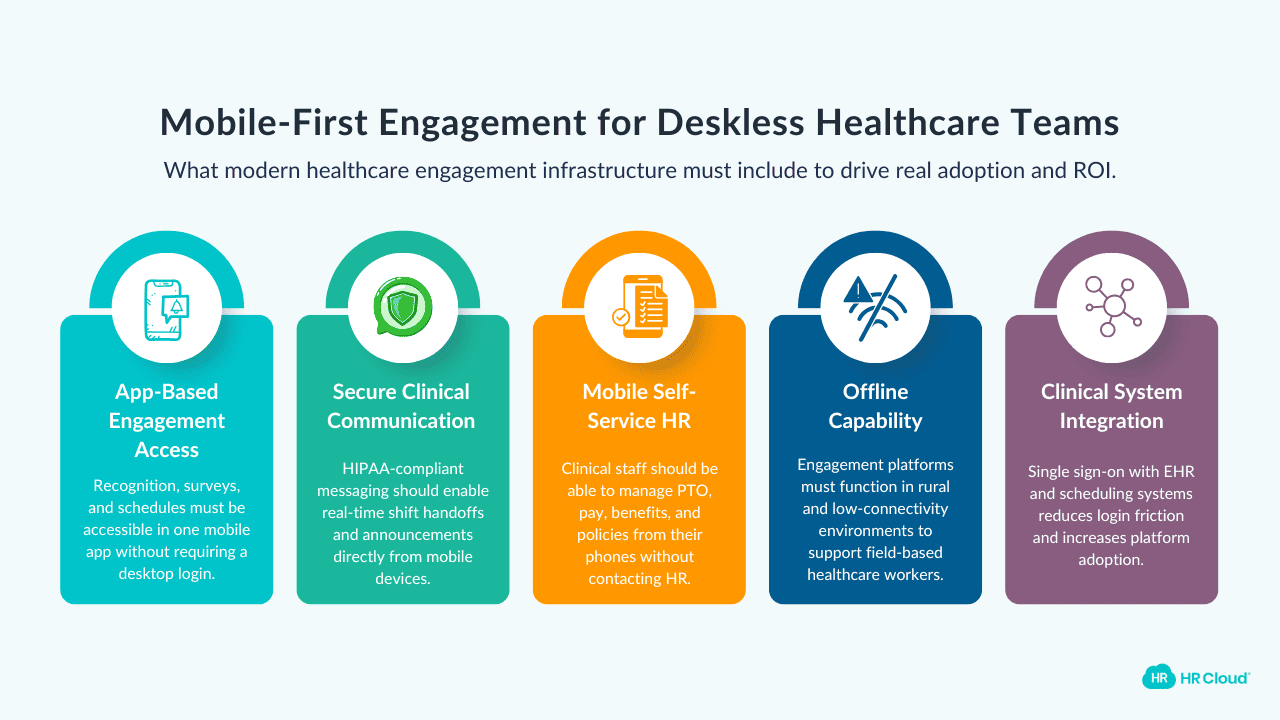
Here's what mobile-first engagement infrastructure actually looks like in a healthcare context:
-
App-based access for recognition, surveys, and schedules. A nurse on a night shift should be able to give a peer a recognition shoutout, complete a two-minute pulse survey, and check her next week's schedule — all from her phone. If your system requires a desktop login, that's not a feature gap. It's an engagement wall.
-
Secure clinical communication tools. HIPAA-compliant messaging platforms that work like the consumer apps your staff already use — quick, intuitive, and mobile — are table stakes in 2026. Shift-to-shift handoffs, real-time announcements, and direct manager communication shouldn't require people to find a desktop or dig through an email inbox.
-
Self-service HR access on mobile. PTO requests, pay stubs, benefits information, policy documents — clinical staff should be able to handle all of this from their phones without calling HR or waiting for a desktop. This respects how their workday actually operates.
-
Offline capability. In rural health systems, home health environments, and certain care facilities, connectivity isn't always reliable. Engagement and onboarding platforms that require constant connectivity lock out field-based and rural clinical workers entirely.
-
Integration with clinical systems. The fewer logins your clinical staff manage, the higher your platform adoption. Single sign-on integration with your EHR and clinical scheduling systems eliminates one of the most common barriers to engagement tool usage among nurses and allied health professionals.
How employee engagement software for healthcare handles these deskless challenges directly affects the ROI from any engagement initiative. Technology isn't the whole answer but the right technology definitely makes every other strategy easier.
Measuring Healthcare Employee Engagement
If you can't measure it, you can't improve it.
That principle applies everywhere and healthcare engagement is no exception. But measuring engagement in a clinical environment requires adaptations that generic HR approaches typically miss.
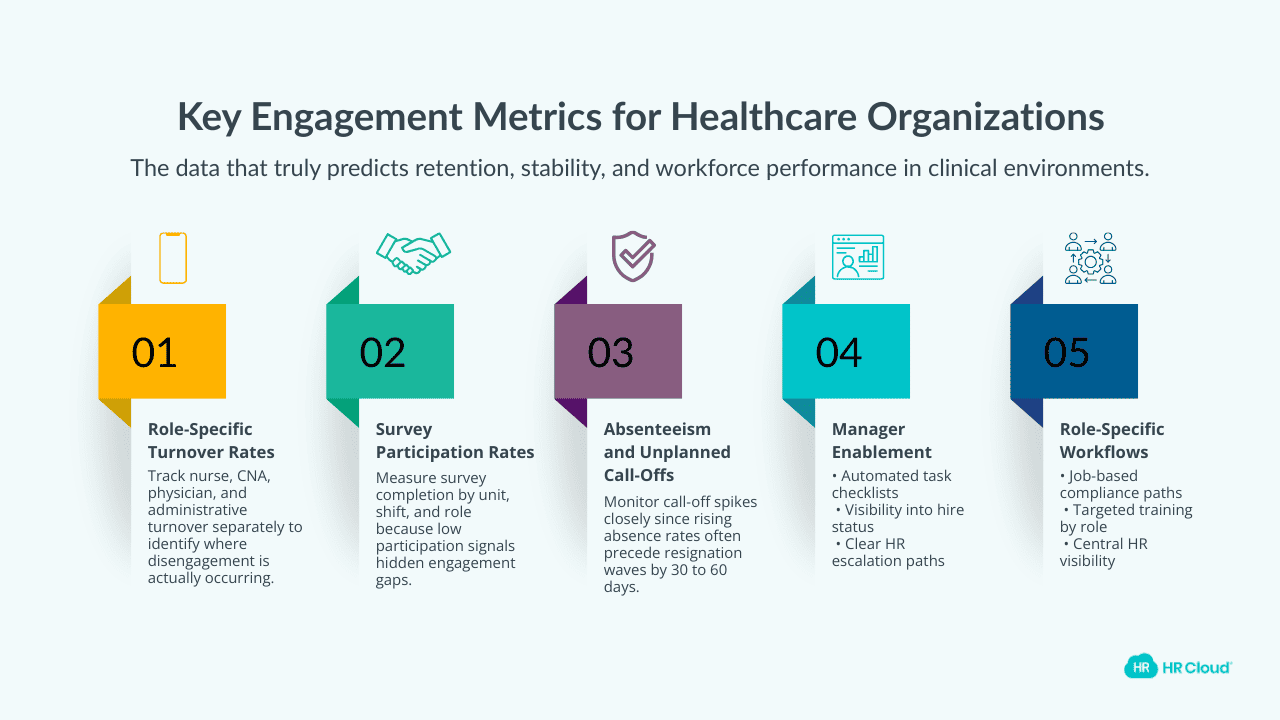
Key Metrics for Healthcare Organisations
The metrics that matter most in healthcare engagement go well beyond annual survey scores. Here's what a comprehensive measurement framework looks like:
-
Turnover rates by role. Aggregate turnover numbers obscure the story. Track nurse, CNA, physician, and administrative turnover separately. SHRM's healthcare workforce research consistently shows that role-specific tracking is the fastest path to targeted intervention.
-
Survey completion rates. If your clinical staff aren't completing engagement surveys, the data you're collecting is biased toward your most engaged employees. Track participation by unit, shift, and role, and treat low completion as a signal worth investigating.
-
Absenteeism and unplanned call-offs. Unplanned absence rates in clinical units are one of the most practical leading indicators of disengagement. When a unit's call-off rate spikes, it often precedes a wave of resignations by 30–60 days.
-
eNPS (Employee Net Promoter Score). One question — "How likely are you to recommend this organisation as a place to work?" — yields surprisingly actionable data when tracked over time and broken down by department or facility.
-
Recognition program participation. How many employees have given or received recognition in the last 30 days? Low participation is a canary in the coal mine for culture problems that surveys might not yet be capturing.
Linking Engagement to Patient Outcomes
If you can link engagement to patient outcomes, you can get management buy-in for the program more easily. The good news is that the research on this linking is robust and growing.
Press Ganey's workforce data shows that hospitals in the top quartile for staff engagement achieve four-star or higher CMS ratings 2.3 times more often than low-engagement facilities. Gallup's healthcare research consistently correlates nurse engagement with HCAHPS patient satisfaction improvements of up to 18%.
Build engagement reporting that maps alongside your clinical outcomes data — readmission rates, patient satisfaction scores, safety incidents. When your CHRO can show the board a dashboard where engagement scores and patient outcomes move in tandem, engagement becomes a strategic investment, not a line item waiting to be cut.
How to Build Healthcare Employee Recognition Programs That Resonate?
Most healthcare organisations have some form of recognition programme. So the problem isn't awareness but operationalization.
A recognition platform that nobody uses, a peer nomination process that requires three approval steps, or a monthly award that the same three people seem to win every quarter do not really help with improving employee engagement.
Building a programme that actually sticks in a clinical environment requires getting four structural elements right.
#1. Design for the shift, not the office.
The single biggest reason healthcare recognition programmes fail is that they were built around day-time availability patterns that don't exist in clinical work. Nomination forms that close on Fridays miss weekend shift staff entirely. Recognition ceremonies scheduled during business hours exclude night shift nurses by default.
Before you choose a platform or design a process, map your workforce's actual shift patterns and build around those.
#2. Set a recognition frequency target and hold managers to it.
Recognition that depends entirely on spontaneous manager initiative will always be inconsistent.
Gallup research suggests that employees who receive meaningful recognition at least once a week show significantly higher engagement and lower safety incident rates than those recognised less frequently.
Turn that into a measurable expectation: every manager recognises at least one team member publicly per week. Track it. Report on it at the unit level. When it drops, treat it as an indicator of engagement going wrong.
#3. Teach managers what good recognition looks like.
Vague recognition — "great job this week" — does nothing. In fact, it signals that the manager wasn't paying close enough attention to name what actually happened.
Train managers to follow a simple structure:
1. name the specific action
2. connect it to its impact on the patient or the team
3. deliver it where colleagues can see it
The DAISY Foundation's recognition model has spread to thousands of healthcare organisations because it enforces exactly this specificity. A DAISY nomination requires a written story, not a checkbox.
#4. Measure participation, not just sentiment.
Annual engagement surveys will tell you whether employees feel recognised in general. They won't tell you whether your recognition programme is working.
Track monthly active participation:
-
how many employees gave recognition
-
how many received recognition
-
how recognition numbers break down by unit, shift, and role.
A unit where 80% of staff gave or received recognition last month has a fundamentally different culture than one where the number is 12%.
A recognition programme that sticks isn't the one with the best technology or the most generous rewards budget. It's the one that's been designed around how your clinical workforce actually operates, with clear expectations for managers and measurement that catches drift before it becomes disengagement.
Segment-Specific Engagement Playbooks
Strategy is essential. But strategy without a starting point is just philosophy. The three playbooks below give you a structured starting point for each care setting with
-
diagnostic questions to gauge where you actually are
-
prioritised actions ranked by impact
-
a phased 90-day timeline
-
metrics to assess whether it's working
Hospital Employee Engagement Playbook
Quick Assessment:
1. What is your 90-day nurse retention rate on your two highest-turnover units, and has it moved in either direction in the last 12 months?
2. Do your charge nurses have a direct, structured channel to give feedback to unit leadership and can you name the last time it was visibly acted on?
3. Can your night and weekend shift staff access your recognition platform from their phones without a desktop login?
4. Does your new hire onboarding differ meaningfully between RNs, allied health professionals, and administrative staff — or is it the same orientation for everyone?
5. When was the last time your HR team reviewed agency staffing spend by unit and correlated it against engagement data?
Priority Actions:
-
Highest impact, start here: Redesign your 90-day onboarding for RNs to include explicit cultural connection milestones alongside clinical competency checkpoints. Introduce a structured peer buddy pairing in the first two weeks. The first 90 days are your highest-leverage retention window — treat them accordingly.
-
Quick win: Audit mobile access to your recognition platform for night and weekend shift staff. If they can't recognise a colleague from their phone during a shift, your recognition programme effectively doesn't exist for 40% of your clinical workforce.
-
Medium-term: Launch a unit-based shared governance pilot in your highest-turnover department. Start with one unit, give nurses genuine decision-making input on scheduling or protocol design, and document what changes. Evidence of impact is what earns the budget to scale it.
90-Day Timeline:
-
Days 1–30: Conduct a brief pulse survey in your two or three highest-turnover units. Focus questions on communication access, recognition visibility, and onboarding experience — not general sentiment. Audit mobile platform access and identify gaps. Review agency staffing by unit to identify your costliest disengagement hotspots.
-
Days 31–60: Redesign RN onboarding for the 90-day framework. Launch the shared governance pilot in one unit. Deploy mobile recognition access fixes identified in month one. Hold one listening session per unit without managers present.
-
Days 61–90: Roll out the revised onboarding framework for all new RN hires. Measure first-30-day engagement indicators for the first cohort through it. Present a unit-level recognition participation report to nursing leadership — make the data visible to the people responsible for culture.
Success Metrics:
-
90-day RN retention rate by unit (target: 5–10 percentage point improvement within two quarters)
-
Agency staffing hours per unit per month versus pre-intervention baseline
-
Recognition platform participation rate for night and weekend shifts specifically
-
Pulse survey completion rate (target: 60%+ among clinical staff)
-
Onboarding satisfaction score at 30 days for new RN cohorts


Multi-Site Clinic Engagement Framework
Quick Assessment:
1. If you pulled engagement or recognition data from your three lowest-performing clinic locations right now, would you be able to identify the specific problem or would you only know that something is wrong?
2. Do your MAs and front-desk staff at satellite locations have identical access to recognition and communication tools as staff at your flagship site?
3. What is the average tenure of an MA across your clinic network? Do you know which locations have the shortest tenure and why?
4. When a new physician joins a satellite clinic, what does their first two weeks look like in terms of team integration (not clinical orientation, but human connection)?
5. Do your clinic managers receive any structured guidance on how to have engagement conversations with their direct reports, or is that left to individual initiative?
Priority Actions:
-
Highest impact, start here: Standardize recognition and communication platform access across every site, including your smallest satellite clinics. Equity of access is the foundation. A clinic where MAs and front-desk staff can't participate in recognition because "that's only set up at the main site" will consistently show lower engagement and higher turnover than its counterparts.
-
Quick win: Create a site-level pulse survey cadence. Say, one short survey per site per quarter, with results shared back to site managers within two weeks. The act of asking and visibly responding does as much engagement work as the data itself.
-
Medium-term: Build a structured new provider integration track — separate from clinical credentialing — for physicians and APPs joining the network. Focus it on team relationships, communication norms, and cultural expectations in the first 30 days. Physician disengagement in multi-site clinic networks is often a belonging problem, not a compensation one.
90-Day Timeline:
-
Days 1–30: Audit platform access across all sites. Identify which locations have gaps in recognition tool deployment, communication channel access, or survey participation. Map MA and front-desk staff tenure by location; this data will tell you more than any survey at this stage.
-
Days 31–60: Close the access gaps identified in month one. Launch site-level pulse surveys at your three lowest-engagement locations first. Brief site managers on how to read and respond to engagement data if they haven't been trained to do this.
-
Days 61–90: Roll out the new provider integration track for all incoming physicians and APPs. Conduct a cross-site recognition participation review. Present the data publicly so high-performing sites are visible and low-performing sites have a clear benchmark to aim for.
Success Metrics:
-
MA 6-month retention rate by site (cross-site parity is the goal — large variance signals a site-level culture problem)
-
Cross-site recognition participation rate (flag any site below 40% monthly active participation)
-
Site-level pulse survey completion rates (target: 55%+ per site per quarter)
-
New provider 90-day satisfaction score
-
Time-to-fill for open MA and front-desk positions by site (sustained vacancies are a leading engagement indicator)
Senior Care Facility Engagement Guide
Quick Assessment:
1. What is your current CNA 90-day retention rate and do you know the most common reason CNAs give for leaving in their first three months?
2. When a CNA raises a concern with a supervisor, what happens next? Is there a visible, consistent response process or does feedback disappear?
3. Do your CNAs work alongside the same residents consistently, or does scheduling rotate them frequently across units and residents?
4. In the last 90 days, has your recognition programme acknowledged anything other than years of service or attendance milestones, specifically moments of exceptional resident care?
5. Does your engagement infrastructure — surveys, recognition, communication — actually function for staff working overnight and weekend shifts, or does it effectively operate Monday to Friday?
Priority Actions:
-
Highest impact, start here: Implement a structured peer mentoring programme for every new CNA in their first 90 days. Pair each new hire with a tenured CNA — not a supervisor — who serves as their first point of contact for real questions. The highest-risk resignation window for CNAs is weeks three through eight, when orientation support has faded but genuine workplace confidence hasn't yet formed. A peer mentor bridges that gap in a way no formal programme can.
-
Quick win: Audit your recognition programme for the last 90 days and count how many recognition moments referenced a specific resident interaction versus a generic operational achievement. If the answer is fewer than 30%, your programme is measuring the wrong things. Redesign your recognition prompts to explicitly invite resident care stories.
-
Medium-term: Create a structured, low-barrier feedback channel for CNAs separate from formal HR processes and accessible to staff without desktop access. A weekly mobile-based question ("What's one thing that made your job harder this week?") with a visible leadership response protocol does more to build trust than an annual engagement survey ever will.
90-Day Timeline:
-
Days 1–30: Review your last three months of CNA exit interview data. If you don't have consistent exit interview data, that's your first action item. Implement a brief mobile exit survey for all departing CNAs immediately. Audit recognition programme content for specificity. Identify your two or three most tenured CNAs per unit who could serve as peer mentors.
-
Days 31–60: Launch the peer mentoring programme for all new CNA hires. Deploy a mobile-first weekly feedback question to all CNAs. Redesign recognition prompts to invite resident care stories. Review scheduling practices — where CNAs are rotated across residents frequently, introduce consistency where operationally possible.
-
Days 61–90: Measure 60-day retention for the first CNA cohort through the peer mentoring programme versus the previous cohort without it. Report recognition programme data to unit managers — volume, specificity, and participation rate. Present the first three months of weekly feedback data to leadership with a visible response plan attached.
Success Metrics:
-
CNA 90-day retention rate (industry baseline: often below 60%; target incremental improvement of 8–12 percentage points within two quarters)
-
CNA 60-day retention rate for peer-mentored versus non-mentored cohorts
-
Percentage of recognition moments referencing specific resident care interactions (target: 50%+)
-
Weekly feedback response rate among CNAs (target: 40%+ within 60 days of launch)
-
Overnight and weekend shift recognition participation rate versus day shift rate (gap of more than 20 percentage points signals an access or culture problem specific to those shifts)
How HR Cloud Supports Healthcare Engagement at Scale
Healthcare HR doesn't need more tools. It needs fewer, better-connected ones. A single system where onboarding, compliance, communication, and recognition reinforce each other rather than compete for attention.
That's exactly the problem HR Cloud was built to solve.
The Workmates engagement module delivers peer recognition, pulse surveys, and team communication in a mobile-first interface clinical staff can access from any device, on any shift. The same platform that automates new hire workflows, I-9 compliance, and licensure tracking also powers the recognition feed. When compliance and culture live in the same system, they stop feeling like opposites.
The results are measurable. Behavioral Progression Inc., a growing behavioral health company, implemented HR Cloud to address a chaotic, paper-based onboarding process that was generating constant friction for new therapists and HR staff alike.
After implementation, they saw:
-
60% reduction in new hire questions
-
therapist onboarding time cut from four weeks to 2.5 weeks
-
20% increase in employee engagement through Workmates
-
10% improvement in therapist retention at the six-month mark.
"The automation features have proven to be valuable assets that streamline the onboarding process and enhance overall efficiency," said Nicole Minard, CEO
For multi-site healthcare organisations, the platform supports site-level configuration within a consistent organisational framework — the same tools, with flexibility to reflect each facility's culture. For systems managing thousands of deskless workers, the mobile app is full-featured, not a desktop tool adapted for phones.
See how HR Cloud's employee engagement software for healthcare works in clinical environments.
Or explore the full Behavioral Progression case study to see the numbers in detail.
The Only Engagement Strategy That Actually Sticks
Employee engagement in healthcare in 2026 determines whether your nurses stay or leave, whether your CNAs connect to purpose or burn out, whether your organisation delivers the care it exists to provide.
The playbooks in this guide won't all apply to every organization as is, and that's by design. Adapt them to your specific context, your specific workforce, and your specific retention pressures.
But whatever you implement, close the feedback loop. If your staff told you night shift workers feel invisible, and 90 days later your mobile recognition data shows that's changed, say that out loud. The visible connection between "we listened" and "we acted" is what turns a programme into a culture.
For additional listening question templates and practical implementation resources, see HR Cloud's guide on how to improve employee engagement in healthcare.
FAQS
What is employee engagement in healthcare?
Employee engagement in healthcare refers to the emotional commitment and connection healthcare workers have to their organisation, patients, and care mission. Engaged healthcare employees demonstrate higher patient satisfaction scores, better safety outcomes, and significantly lower turnover rates compared to disengaged staff.
Why is employee engagement important in healthcare?
Employee engagement in healthcare directly impacts patient outcomes, safety, and organisational performance. Engaged healthcare workers provide better patient care, fewer medical errors, and lower readmission rates. Financially, engagement reduces costly turnover (RN replacement costs $52,000–$64,000) and decreases reliance on expensive agency staffing.
How do you improve employee engagement in healthcare?
To improve employee engagement in healthcare:
-
integrate engagement with onboarding and compliance processes
-
implement mobile-first communication tools for deskless clinical workers
-
create segment-specific strategies for hospitals, clinics, and senior care facilities
-
establish peer recognition programmes tied to patient care outcomes
-
conduct regular pulse surveys and act on feedback
-
provide clear career development pathways for clinical staff.
How do you measure employee engagement in healthcare?
You can measure healthcare employee engagement through annual engagement surveys and quarterly pulse surveys; role-specific turnover rates (RN, CNA, physician); absenteeism and unplanned call-off rates; participation rates in recognition programmes and surveys; eNPS (Employee Net Promoter Score); and patient outcome correlations — HCAHPS scores, safety incidents, readmission rates. Linking engagement metrics to patient care quality is essential for C-suite buy-in.
What are effective healthcare employee recognition programmes?
Effective healthcare recognition programmes include: peer-to-peer recognition allowing clinical staff to recognise colleagues in real time; patient-centred recognition celebrating positive patient outcomes; values-based recognition tied to organisational mission; milestone recognition for certifications and clinical achievements; team-based recognition for units or departments; and mobile-accessible platforms enabling recognition during shifts. Recognition should be frequent, specific, and tied to patient care excellence.
How do you engage deskless healthcare workers?
Engage deskless healthcare workers through: mobile-first engagement platforms accessible via smartphone apps; shift-based communication tools for announcements and recognition; self-service HR access for schedules, PTO, and pay stubs; microlearning for compliance training during breaks; offline capability for areas with poor connectivity; and integration with clinical systems for single sign-on. The goal is a system that works for 12-hour shift workers without computer access.

Keep Reading
How to Use AI in HR: Moving From Drafts to Trackable Workflows Across the Full Lifecycle
You're an HR director at a 400-person company. You have three open requisitions, a
7 Signs Your HR Team Needs Better HRIS Software in 2026
You didn't set out to build a patchwork of spreadsheets, workarounds, and disconnected
HR Transformation in 2026: What Mid-Market HR Teams Are Prioritizing This Year
You're an HR Director at a 700-person company, managing 30% more headcount than you had
Like What You Hear?
We'd love to chat with you more about how HR Cloud® can support your business's HR needs. Book Your Free Demo

Build a Culture of Recognition. Boost Engagement. Guaranteed.
Workmates empowers employees to stay informed, connected, and appreciated—whether they’re on the front line, in the office, or remote. Recognition drives 12x higher engagement.Trusted by industry leaders in every sector




Cut Onboarding Costs by 60%.
Take the confusion and follow-ups out of onboarding with automated workflows, digital forms, and structured portals—so new hires ramp faster 3X quicker.Trusted by industry leaders in every sector