Healthcare HR Compliance: The 2026 Checklist Every HR Team Needs

- The Joint Commission's Accreditation 360: What Changed and Why It Matters
- I-9 and E-Verify Compliance
- Credential and License Tracking
- HIPAA Workforce Compliance
- OSHA Compliance for Healthcare Settings
- Workforce Documentation: The Audit-Ready Standard
- Contingent and Agency Workforce Compliance
- The 2026 Healthcare HR Compliance Checklist
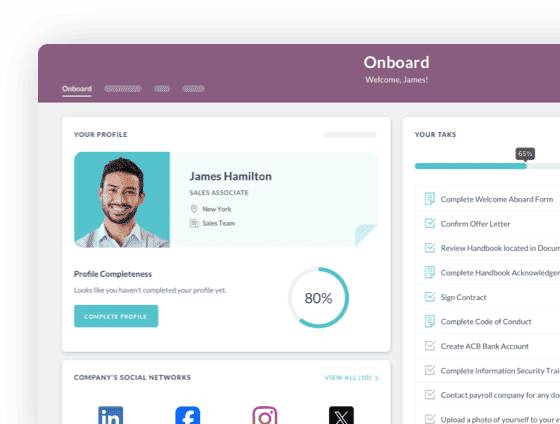

 Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.
Cut onboarding time
by 60%—here's the
Ultimate Checklist
that helped do it.

Healthcare HR compliance is complex and constantly evolving, making a structured checklist essential for staying audit-ready in 2026. This blog outlines key compliance areas including hiring documentation, credential tracking, labor laws, and healthcare-specific regulations like HIPAA and workplace safety. It highlights actionable steps such as maintaining accurate records, automating compliance workflows, and conducting regular audits to prevent risks. By following a comprehensive checklist, HR teams can reduce legal exposure, ensure continuous compliance, and maintain smooth, disruption-free healthcare operations.
2026 brought the most significant overhaul of healthcare accreditation standards in years, with The Joint Commission rewriting the rules on staffing, documentation, and competency validation. This checklist walks healthcare HR teams through every major healthcare HR compliance requirement (I-9 and E-Verify, Joint Commission National Performance Goals, HIPAA, OSHA) and shows how purpose-built HR systems reduce the risk of getting caught off-guard.
Key Takeaways
-
The Joint Commission's Accreditation 360 restructuring took effect January 1, 2026, replacing National Patient Safety Goals with National Performance Goals. Nurse staffing is now embedded directly in accreditation for the first time.
-
I-9 fines range from $288 to $2,861 per form, and ICE has resumed aggressive worksite enforcement with AI-assisted audit tools targeting high-turnover sectors.
-
HIPAA workforce compliance penalties are adjusted annually. The most recent update was published in the Federal Register on January 28, 2026.
-
Credential gaps are no longer just a paperwork problem. Under NPG Goal 12, they are a documented patient safety risk reviewable during surveys.
-
Most compliance failures in healthcare trace back to manual processes, missed expiration reminders, and fragmented recordkeeping. Not bad intentions. HR Cloud's healthcare onboarding and retention guide covers how structured compliance workflows also improve retention.
Introduction
"We knew the license was expiring. We just didn't have anyone tracking it."
That's the sentence no compliance officer wants to say in a Joint Commission exit interview. But it plays out constantly — across hospitals, home health agencies, and outpatient clinics — because credential tracking still lives in spreadsheets, shared drives, and someone's mental to-do list.
2026 changed the stakes considerably. The Joint Commission rolled out its biggest structural overhaul in recent memory. CMS updated enforcement priorities. ICE worksite enforcement using AI-assisted flagging is active. And nurse staffing is now formally embedded in accreditation standards as a measurable patient safety requirement, something that has never happened before.
This healthcare HR compliance checklist covers the regulatory landscape your team needs to navigate, the specific areas where documentation gaps create the most risk, and how the right healthcare HR compliance software can shift compliance from reactive scrambling to something that actually runs in the background. For a broader look at where healthcare HR is heading, HR Cloud's industry page for healthcare covers the full scope of what modern HR platforms need to handle.
1. The Joint Commission's Accreditation 360: What Changed and Why It Matters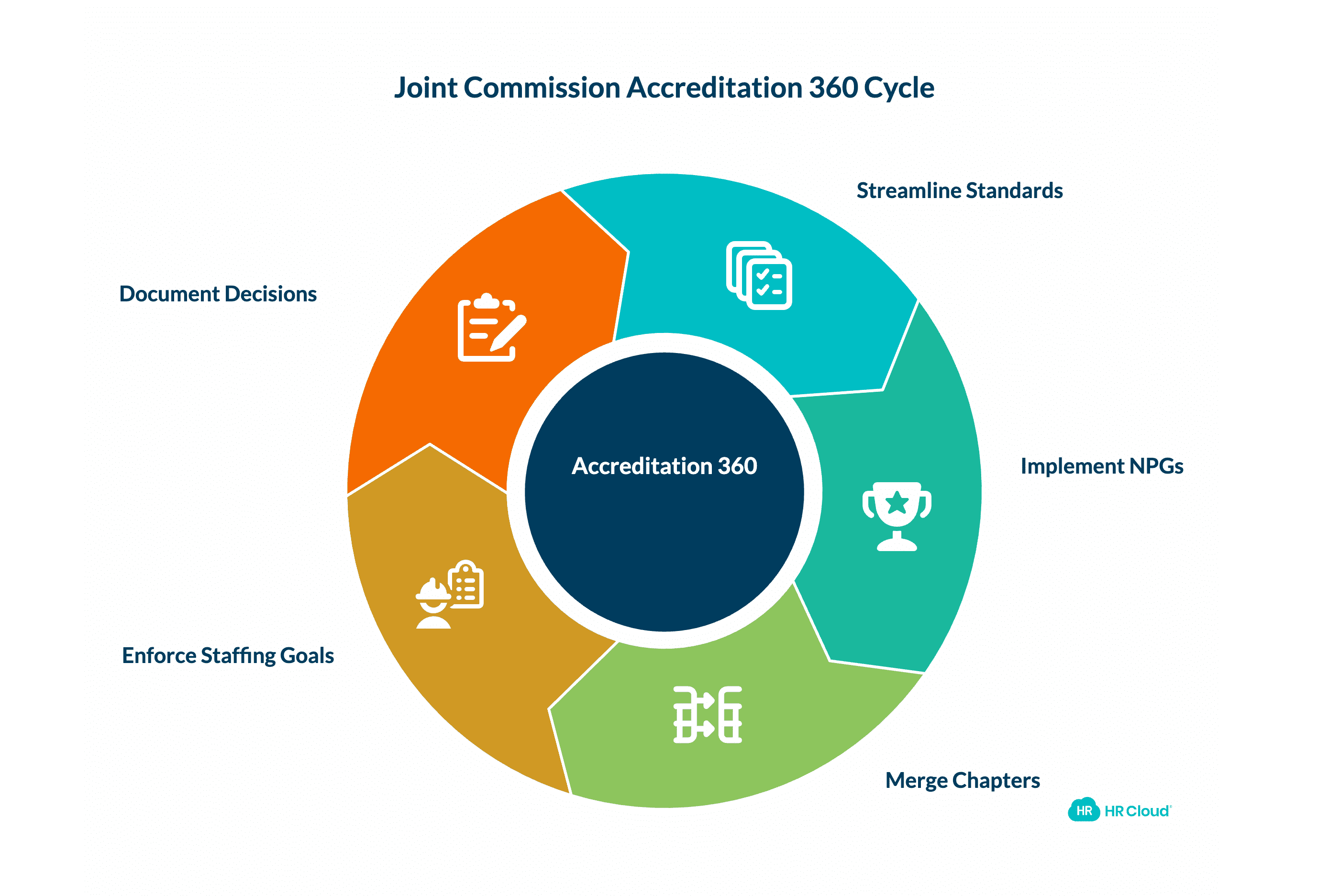
What happened
On January 1, 2026, The Joint Commission's Accreditation 360 restructuring took effect. The total number of standards dropped from 1,551 to 774, but as JC clarified, no new requirements were introduced. Existing standards were streamlined and renumbered to more clearly separate CMS Conditions of Participation from JC-specific requirements.
Key structural changes healthcare HR teams need to understand:
The old "National Patient Safety Goals" chapter is gone. In its place is the new "National Performance Goals" (NPG) chapter. This matters because the NPG framework elevates certain topics to a higher level of accountability — and two of those topics are suicide risk reduction and nurse staffing.
The Environment of Care and Life Safety chapters were merged into a single "Physical Environment" chapter, with elements of performance reduced by roughly 47% for hospitals. Fewer line items, but the underlying requirements remain.
NPG Goal 12: Staffing as a patient safety metric
This is the most significant HR-specific change in 2026. Beginning January 1, 2026, The Joint Commission enforces National Performance Goal 12: Health Professional Resource Management. Hospitals must now demonstrate they are staffed to meet patient needs and that staff are competent to provide safe, quality care.
Under NPG Goal 12, that means a clearly defined staffing plan aligned to patient needs, documented executive oversight, and evidence that staffing decisions are data-driven and defensible.
Surveyors won't ask whether you hit a specific ratio. They will ask whether you can prove your decisions were intentional and documented. Common exposure areas include inconsistent documentation of competency validation, lack of proof that staffing plans are actively monitored, weak orientation documentation for float or agency staff, and missing or outdated licensure verification. That last one is squarely in HR's domain.
|
What Surveyors Will Evaluate |
What HR Needs to Provide |
|
Staffing adequacy tied to patient acuity |
Role-based staffing documentation |
|
Competency validation |
Training completion records, credential files |
|
Executive oversight |
Named accountability, documented review cadence |
|
Float and agency staff orientation |
Orientation records for contingent workers |
|
Licensure currency |
Active license verification with timestamps |
For a practical look at how top healthcare HR challenges map to documentation requirements, see HR Cloud's guide to top healthcare HR challenges in 2025.
2. I-9 and E-Verify Compliance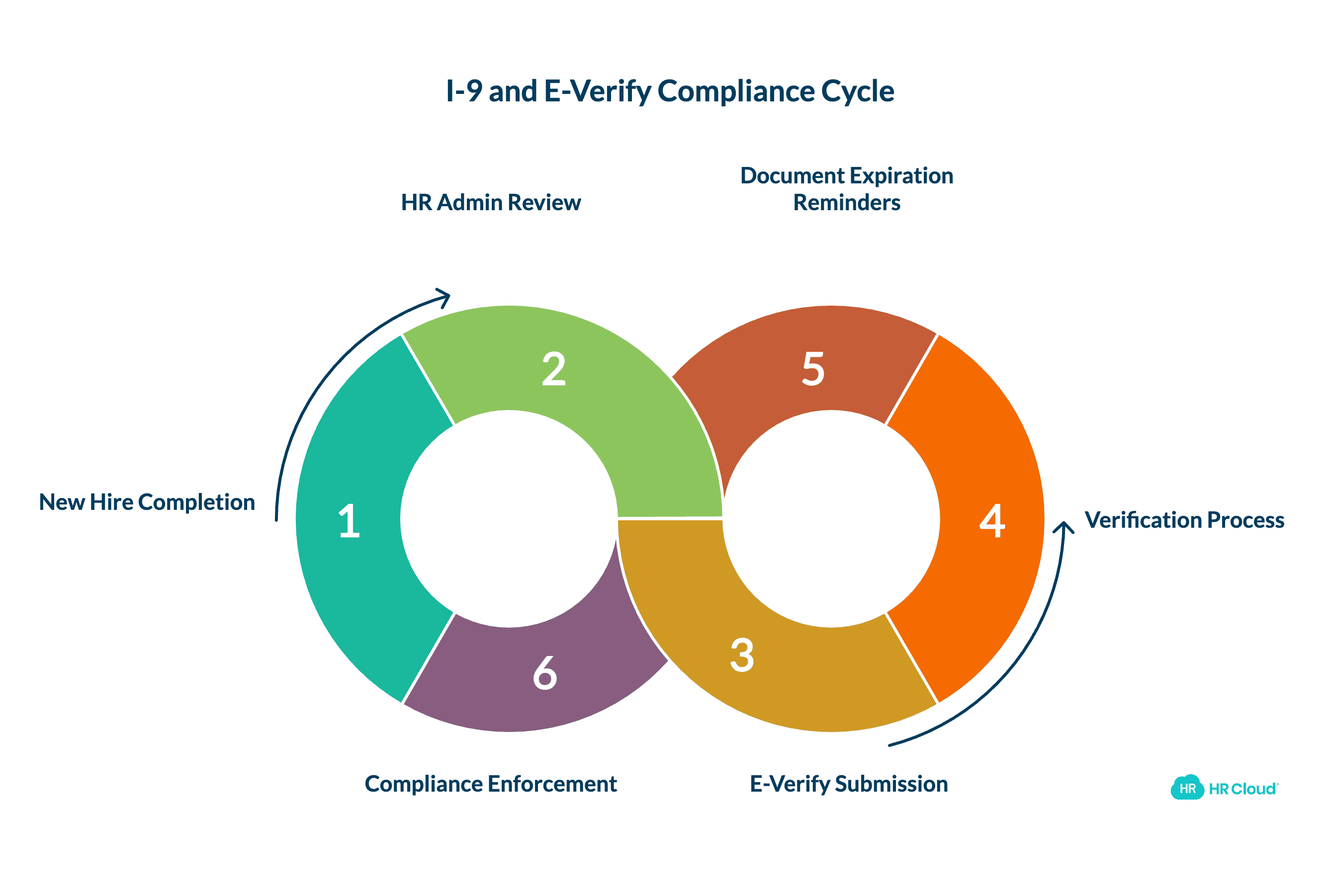
Healthcare is one of the highest-turnover industries in the U.S. That creates a specific I-9 compliance problem: volume. Each new hire requires Form I-9 completion within three business days of their start date. When an organization processes dozens of hires monthly across multiple facilities, the margin for error compounds fast.
What's current in 2026
The updated Form I-9 (edition date 01/20/25) is now required, valid through May 31, 2027. It includes minor language changes and an updated privacy notice. If your organization is still using older versions, that is an immediate fix. USCIS I-9 Central maintains the current accepted versions and updates employers on any changes.
ICE has resumed aggressive worksite enforcement using AI tools to flag I-9 discrepancies across high-turnover sectors. Healthcare is explicitly on that list.
Fines for I-9 violations run from $288 to $2,861 per form. For a hospital hiring 200 nurses a year with a 5% error rate, that adds up quickly, and that's before any escalation for repeat violations.
Why This Matters for Multi-Facility Teams: When HR is managing bulk healthcare onboarding across multiple sites, manual I-9 tracking creates the exact gaps ICE is looking for. Errors cluster during high-volume hiring periods when teams are moving fast. Automated workflows reduce that risk by enforcing the same sequence regardless of hiring volume.
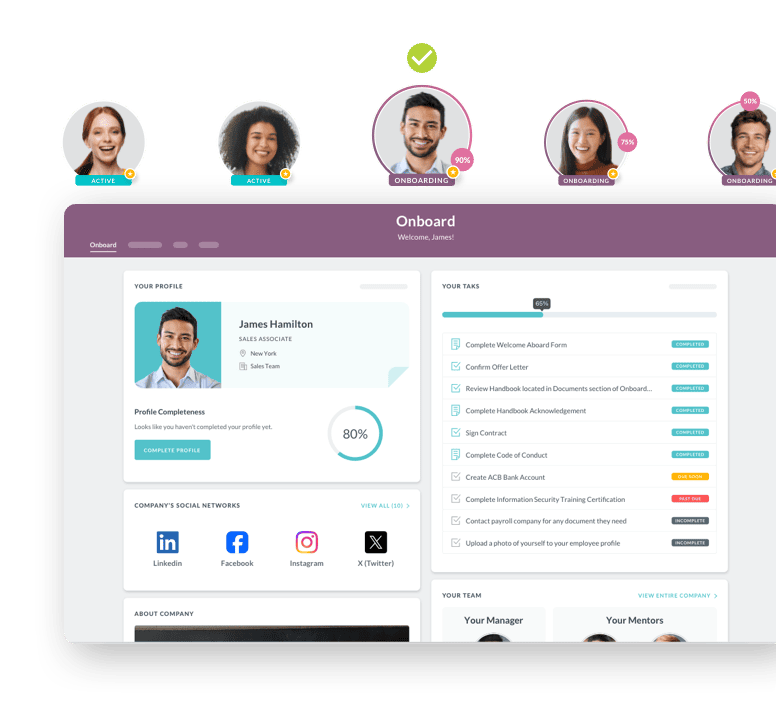
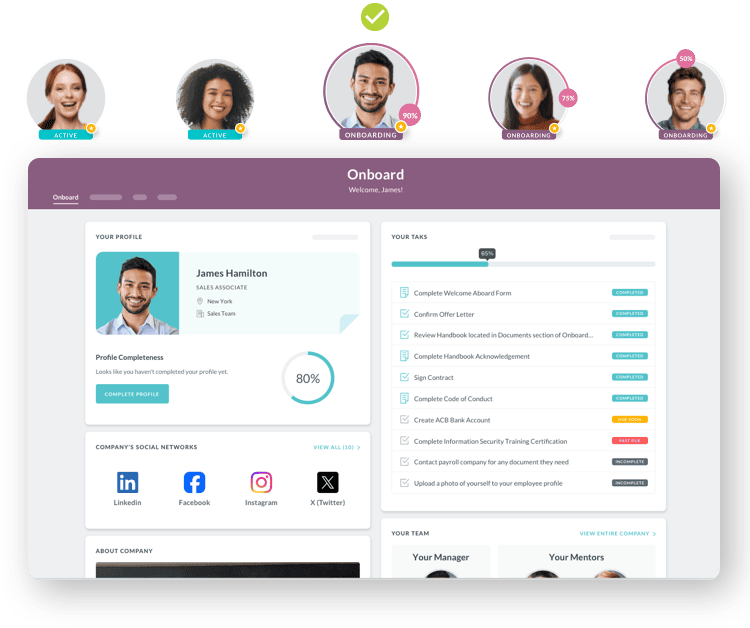
E-Verify and automated workflows
HR Cloud integrates directly with E-Verify as part of the I-9 workflow. Once an employee completes their portion of the I-9, the HR admin finishes the employer section and submits the case to E-Verify without leaving the platform. All past and current E-Verify cases track under a single tab in the Onboard application. For teams managing verification across multiple facilities, that centralized audit trail eliminates the scattered email threads and manual logs that make audits stressful.
HR Cloud also supports I-9 document expiration reminders. The system sends automated alerts 7 days before I-9 documents expire, covering work authorization, identity and employment authorization documents, and reverification documents. That proactive notification catches issues before they become findings.


3. Credential and License Tracking
If there is one area where manual processes most reliably fail healthcare organizations, credential tracking is it.
A nurse's license expires. No one noticed. She works two more shifts. Now there is a Joint Commission finding, a potential billing suspension, and a credentialing gap on record. This is not a hypothetical — it happens because credential tracking gets treated as an administrative task rather than a compliance system. The distinction matters when surveyors arrive. For organizations dealing with high-volume clinical hiring, HR Cloud's healthcare onboarding guide shows how credential workflows integrate into the full new hire experience.
The 2026 credential compliance checklist
Primary licenses (nursing, therapy, physician)
-
Active license status verified at hire via primary source, not self-reported
-
Expiration dates logged with automated renewal alerts
-
Verification documented and retrievable per employee
Certifications (BLS, ACLS, specialty certifications)
-
Stored in employee profile, not email folders or shared drives
-
Renewal workflows triggered before expiration, not on it
Background checks
-
Completed before or at onboarding, not after start date
-
OIG exclusion list screening documented at hire
-
Sanctions checks for travel nurses, per diem, and locum providers
Immunization and health records
-
TB test, flu vaccination, and role-specific health requirements tracked with expiration visibility
HR Cloud's Onboard platform supports healthcare credential tracking workflows through document request tasks, chained tasks that enforce completion sequence, Checkr background check integration, and role-based document access controls. Document request tasks let HR configure exactly which credentials each role needs to upload — a pediatric therapist's checklist looks different from a billing coordinator's — and the system flags incomplete items rather than waiting for someone to notice.
4. HIPAA Workforce Compliance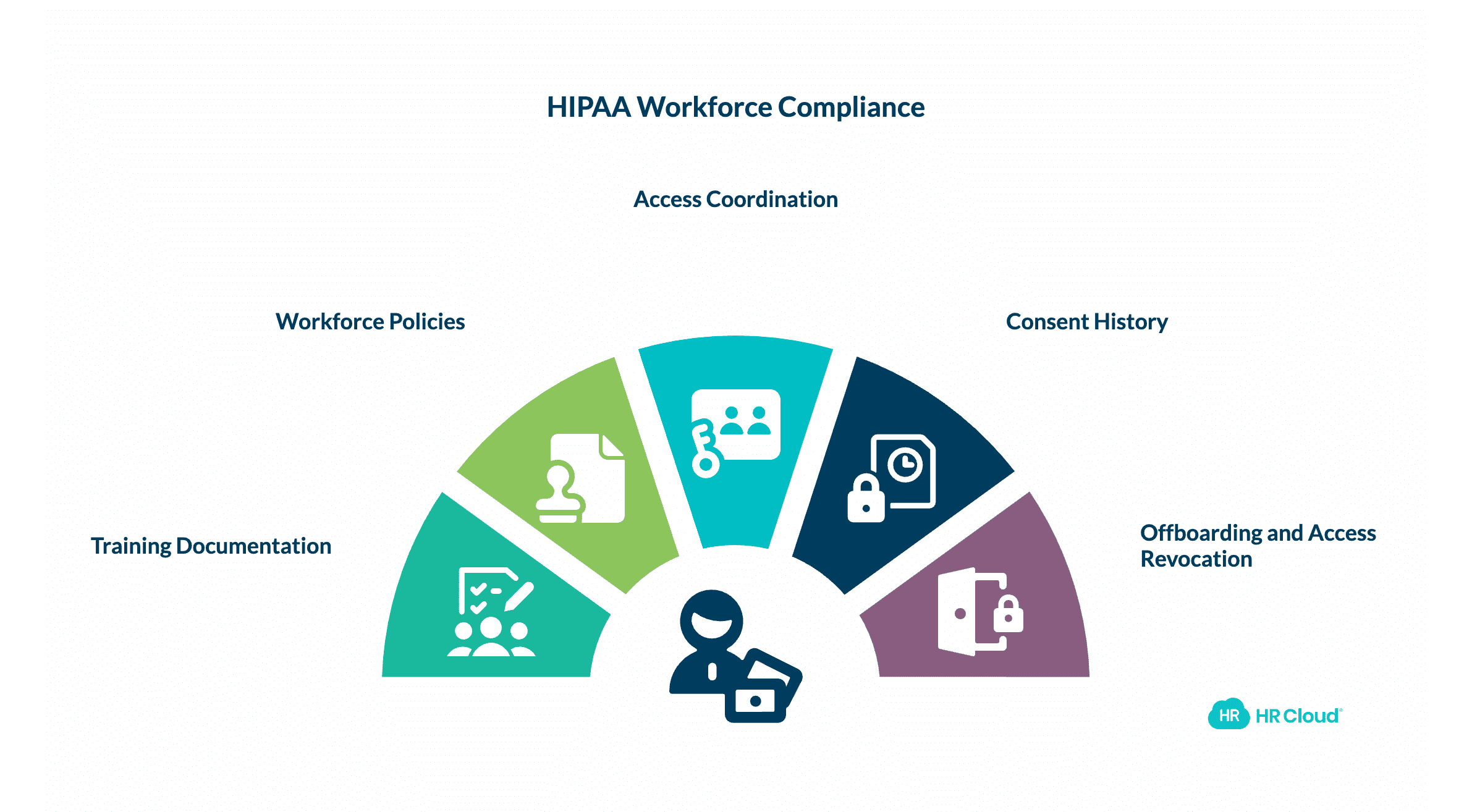
HIPAA compliance has an employee dimension that's separate from the patient privacy side, and it's frequently under-managed.
Most protected health information breaches result from employee negligence and noncompliance with HIPAA regulations rather than external hacking. That is a training and documentation failure, not a technology failure. HIPAA penalty amounts are adjusted annually for inflation; the most recent update was published in the Federal Register on January 28, 2026.
What healthcare HR is responsible for
-
Training documentation. Annual HIPAA training must be documented per employee, with completion records retained. Refresher training is required when policies change materially, and those completions need records too.
-
Workforce policies. Written policies on PHI handling must exist, and employees must acknowledge them with a timestamp.
-
Access coordination. Role-based access to clinical systems should be tied to job function. HR coordinates provisioning when employees are hired, transferred, or terminated. This is an HR workflow responsibility — the PHI system controls themselves sit with IT and the EHR vendor.
-
Consent history. HR Cloud's task system tracks training completion with timestamped records per employee. Healthcare organizations can use that audit trail to demonstrate HIPAA training was assigned, completed, and documented when a compliance question surfaces.
-
Offboarding and access revocation. PHI access should be revoked on or before an employee's last day. This is a persistent gap in organizations without
structured offboarding workflows. This is a persistent gap in organizations without structured offboarding workflows.
Manual vs. automated workforce training documentation
|
Documentation Area |
Manual Approach |
Automated Approach |
|
Training completion records |
Spreadsheet or binder, manually updated |
Timestamped per-employee record, always current |
|
Policy acknowledgments |
Emailed form, filed inconsistently |
Digital signature with timestamp, audit-ready |
|
Consent history |
No centralized record |
Accessible in settings, timestamped by employee |
|
Access revocation at termination |
Checklist item, easy to miss |
Triggered automatically on offboarding |
|
OCR investigation response |
Hours of record gathering |
Retrievable on demand |
Many healthcare organizations complete HIPAA training. Fewer can prove it on demand. When an OCR investigation opens, the question is not "do you do training?" It is "show me the records for these 47 employees going back three years." If documentation lives in a binder or shared drive with inconsistent naming conventions, the audit becomes expensive regardless of whether the underlying training happened.
5. OSHA Compliance for Healthcare Settings
Healthcare workers face occupational hazards that most industries don't. Bloodborne pathogens. Hazardous chemicals. Workplace violence. OSHA standards for healthcare are specific, and the documentation requirements are their own category of administrative work.
In January 2025, OSHA terminated the COVID-19 healthcare rulemaking and is now focused on a broader infectious diseases standard for healthcare settings. OSHA can still enforce COVID-19 protections under the General Duty Clause and existing PPE and Respiratory Protection standards.
Core OSHA documentation requirements for healthcare HR
|
Standard |
Key HR Documentation Requirements |
|
Bloodborne Pathogens |
Exposure Control Plan (annually reviewed), training records for all exposed workers, Sharps Injury Log |
|
Hazard Communication (2024 GHS update) |
Current Safety Data Sheets accessible, employee training records updated per your facility's compliance timeline (employer training deadline: July 2026) |
|
Personal Protective Equipment |
PPE availability by role documented, proper use training recorded |
|
Workplace Violence Prevention |
Incident reporting process documented, training records maintained |
The penalties for OSHA violations are adjusted annually. OSHA has authority to issue instance-by-instance citations, meaning each individual documentation gap can be cited separately rather than as a single violation.
HR Cloud's task system supports OSHA compliance documentation through configurable checklists, mandatory task workflows, and recurring checklist scheduling. Annual training requirements — bloodborne pathogens, hazard communication, workplace violence — can be set up as recurring checklists that automatically assign to the right employees at the right intervals. Completed tasks generate an audit trail. Overdue tasks trigger alerts before deadlines pass. The same system handles nurse onboarding compliance and medical practice HR workflows with the same underlying task architecture.
6. Workforce Documentation: The Audit-Ready Standard
This section is not about a specific regulation. It is about the operational reality that connects all of them.
Healthcare organizations get audited. Joint Commission surveys. CMS surveys. OCR investigations. ICE worksite visits. State licensing board reviews. Each demands specific documents for specific employees covering specific time periods.
The organizations that handle audits cleanly aren't necessarily the most compliant ones. They're the ones whose documentation is findable, organized, and complete, where compliance breakdowns surface during routine operations rather than during a survey exit meeting.
What audit-ready healthcare HR documentation looks like
Employee files
-
Offer letter, job description, and employment agreement
-
I-9 and E-Verify case record
-
All credentials with expiration dates and renewal history
-
Background check results
-
Training completion records (HIPAA, OSHA, role-specific)
-
Performance reviews
-
Policy acknowledgments with timestamps
Onboarding records
-
Onboarding checklist completion status per employee
-
Form completion dates (I-9 date matters legally; must be within 3 business days)
-
Consent records for privacy policies and terms
-
Document upload records for required credentials
Ongoing compliance records
-
Annual training completions with timestamps
-
License renewal verifications by employee
-
Recurring safety training records
HR Cloud tracks every signature, upload, and task completion as a timestamped audit log. For organizations managing multiple facilities, queue dashboards provide real-time visibility into onboarding progress by site, department, or role — so compliance managers see issues before they become findings, not during a survey.
At All About Kids, a 1,200-employee pediatric therapy provider, a paper-based onboarding process meant "important documentation slipping through the cracks." After switching to HR Cloud, they automated documentation tasks and gained full visibility — their team described it as "nothing is ever missed." At Behavioral Progression, Inc., therapist onboarding time dropped from four weeks to 2.5 weeks, with HR completing tasks three times faster. For teams still building out their processes, free onboarding checklists and templates provide a practical starting point, and the employee offboarding checklist ensures the compliance trail stays complete through separation.
7. Contingent and Agency Workforce Compliance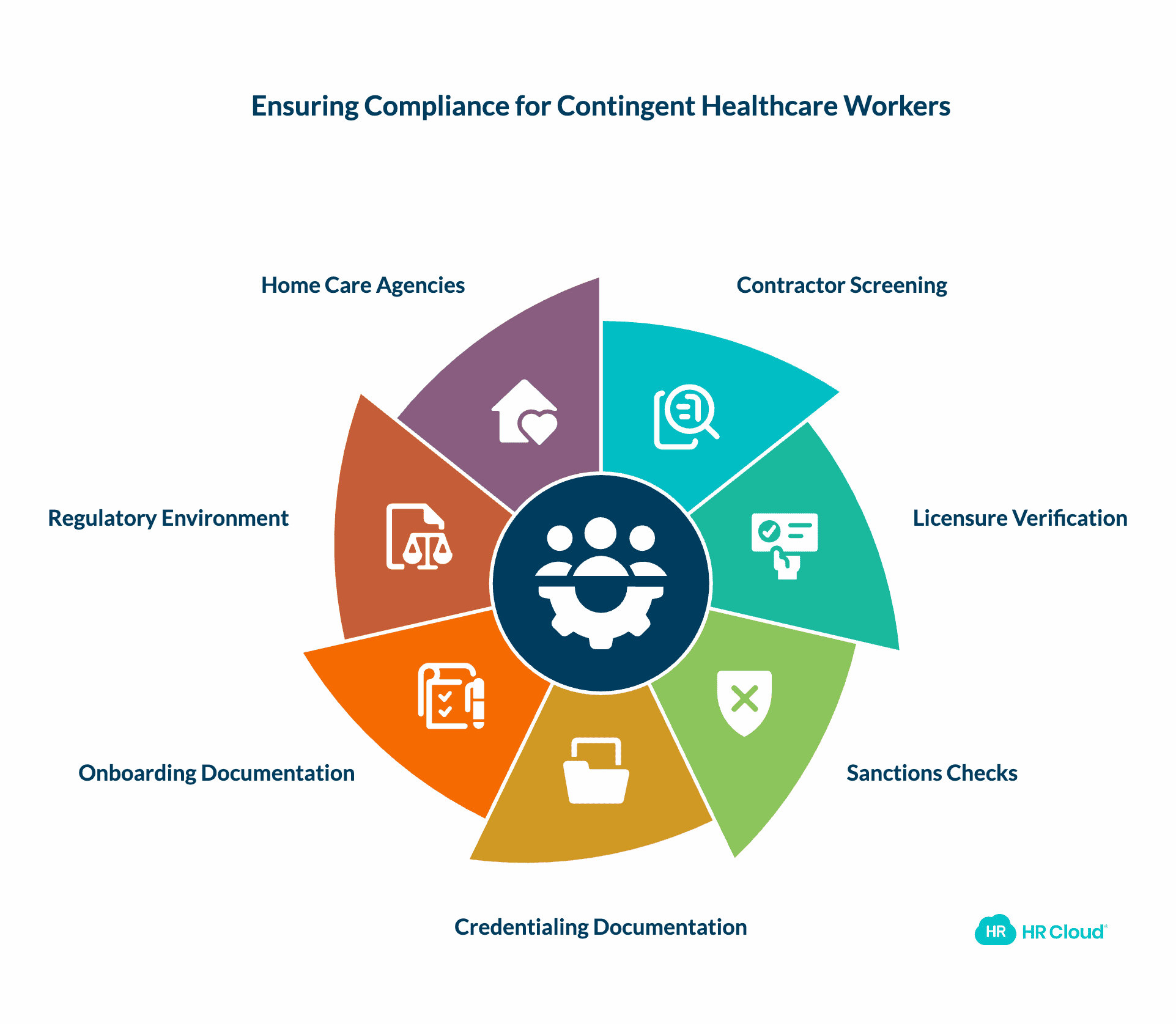
Travel nurses, per diem staff, and locum providers now represent a significant portion of the healthcare workforce. They also carry specific compliance exposure that is frequently under-managed.
Reliance on staffing agencies doesn't outsource liability. Healthcare organizations must validate contractor screening, licensure verification, sanctions checks, and credentialing documentation for every contingent worker, not just employees on payroll.
Under NPG Goal 12, weak orientation documentation for float or agency staff is explicitly identified as a common survey exposure area. The same credential and training requirements that apply to permanent staff must be documented for contingent workers, and those records must be as retrievable as any employee file.
The practical implication: your healthcare onboarding platform needs to handle contingent worker workflows. Checklists configured for agency staff, credential uploads required before a first shift, background check integration that covers contractors. If your current system treats contingent workers as edge cases, 2026's regulatory environment has made that an audit risk. For a closer look at how caregiver turnover in home-based care drives compliance gaps, HR Cloud's guide covers the connection between workforce instability and documentation failures.
For home care agencies dealing with high caregiver turnover — 75% annually per the 2025 Activated Insights Benchmarking Report — this is especially pressing. Every new hire, including per diem and occasional-shift caregivers, needs the same compliance documentation trail as a full-time employee. Reducing caregiver no-shows and improving caregiver retention both start with structured onboarding that captures the right documentation from day one.
Related: Home health HR software and workforce compliance → hrcloud.com/home-health-hr-software
8. The 2026 Healthcare HR Compliance Checklist
Use this as a working framework, not a one-time review. Healthcare organizations face ongoing regulatory updates — what's sufficient today may need adjustment when new OSHA standards finalize or when CMS updates Conditions of Participation. For multi-facility organizations, the 80/20 onboarding framework (80% standardized compliance requirements across all sites, 20% local customization) provides a practical model for maintaining consistency without losing local flexibility. Teams dealing with common onboarding problems in healthcare can find solutions mapped to each challenge type.
I-9 and Work Authorization
-
Updated Form I-9 (01/20/25 edition) in use for all new hires
-
I-9 completed within 3 business days of start date
-
E-Verify cases submitted and tracked centrally
-
I-9 document expiration reminders configured
-
Reverification process documented for temporary work authorization
Licensure and Credentialing
-
Primary source verification completed at hire for all licensed roles
-
License expiration dates logged with automated renewal alerts
-
OIG exclusion list screening documented at hire
-
Credential records maintained per employee profile
-
Contingent worker credentials tracked with same rigor as permanent staff
Background Checks
-
Background check completed before or at start date
-
Screening package appropriate to role (clinical vs. administrative)
-
Results documented in employee file with retrievable audit trail
HIPAA Training and Documentation
-
Initial HIPAA training completed before PHI access
-
Annual refresher training assigned and completion documented per employee
-
Training records retained and retrievable
-
Policy acknowledgments timestamped
-
Offboarding includes PHI access revocation on or before last day
OSHA Safety Training
-
Bloodborne pathogens training documented annually for all exposed workers
-
Hazard communication training updated for 2024 GHS alignment
-
PPE training documented by role
-
Workplace violence prevention training documented where applicable
-
Exposure Control Plan reviewed annually
Joint Commission / NPG Goal 12
-
Staffing plans documented and linked to patient acuity data
-
Competency validation records maintained by role
-
Executive oversight of staffing documented with review cadence
-
Float and agency staff orientation records current and retrievable
General Recordkeeping
-
Consent history accessible and auditable
-
Onboarding checklist completion tracked per employee with timestamps
-
Offboarding triggers credential archive and system access revocation
 Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Discover how our HR solutions streamline onboarding, boost employee engagement, and simplify HR management
Frequently Asked Questions
What is the most significant healthcare HR compliance change in 2026?
The Joint Commission's National Performance Goal 12, effective January 1, 2026, is the most operationally significant shift for healthcare HR teams. It embeds nurse staffing into accreditation as a measurable patient safety metric for the first time, requiring documented staffing plans, competency validation, and executive oversight. Surveyors now evaluate staffing governance, not just headcount.
What are the I-9 compliance penalties for healthcare organizations in 2026?
I-9 fines range from $288 to $2,861 per form depending on violation severity and pattern. Healthcare organizations process high hiring volumes, so even a modest error rate compounds quickly. ICE has resumed worksite enforcement using AI tools specifically targeting high-turnover industries, with healthcare explicitly in scope. See HR Cloud's I-9 and E-Verify compliance guide for healthcare for a detailed breakdown of current enforcement priorities.
How often must HIPAA workforce training be documented?
HIPAA requires initial training before PHI access and refresher training whenever policies change materially. Annual refresher training is widely considered best practice and expected by OCR auditors. All training completions must be documented per employee and retained for a minimum of six years under the HIPAA Security Rule's administrative safeguard requirements.
Does NPG Goal 12 require specific nurse-to-patient ratios?
No. NPG Goal 12 requires hospitals to document that staffing decisions are aligned to patient acuity and clinical needs with executive oversight. The standard evaluates staffing governance and documentation quality, not a fixed numeric threshold. The absence of ratios doesn't reduce documentation burden; it increases it.
What credential records does The Joint Commission expect for agency and travel nurses?
Survey expectations for contingent clinical workers mirror permanent staff requirements: active license verification, primary source documentation, OIG exclusion screening, and scope-of-practice documentation. Weak orientation documentation for float or agency staff is explicitly identified as a common exposure area under NPG standards.
What is the difference between I-9 and E-Verify in healthcare compliance?
Form I-9 is required for every U.S. employer and every hire. It verifies identity and work authorization. E-Verify is a federal system that cross-references I-9 data against government databases electronically. In healthcare, integrating both into a single onboarding workflow (rather than managing them separately) reduces errors and creates a centralized audit trail across high-volume hiring.
What should healthcare HR teams prioritize for Joint Commission survey readiness?
Focus on documentation retrievability, not just documentation existence. Three areas carry the most survey risk: licensure currency for all clinical staff including contingent workers, competency validation records by role, and orientation documentation for float and agency staff. A comprehensive nurse onboarding checklist that builds these requirements into day-one workflows removes the pre-survey scramble.
How does HR Cloud support healthcare HR compliance requirements?
HR Cloud's Onboard platform supports I-9 and E-Verify integration, document request workflows for credential collection, Checkr background check integration, chained tasks for sequenced compliance steps, automated expiration reminders, and role-based document access controls. Every task completion, form signature, and document upload creates a timestamped audit-trail record retrievable for survey preparation or regulatory inquiries. Organizations in medical practice, hospital, and home health settings use the same underlying platform with configurations tailored to each care setting.
Healthcare HR compliance in 2026 demands more than good intentions. It demands systems that track, remind, sequence, and document — automatically. If your current processes rely on spreadsheets, email reminders, and institutional memory, this year's regulatory environment is a practical reason to change that.
See how HR Cloud supports healthcare HR compliance → hrcloud.com/hr-software-for-healthcare

Keep Reading
Healthcare HR Compliance: The 2026 Checklist Every HR Team Needs
2026 brought the most significant overhaul of healthcare accreditation standards in
I-9 and E-Verify for Healthcare Organizations: Complete Compliance Guide for 2026
Healthcare organizations face unique I-9 compliance challenges due to high turnover rates
Why Compliance and Engagement Must Work Together in Healthcare HR
Picture your most experienced RN. She's twelve hours into a shift when she receives her
Like What You Hear?
We'd love to chat with you more about how HR Cloud® can support your business's HR needs. Book Your Free Demo

Build a Culture of Recognition. Boost Engagement. Guaranteed.
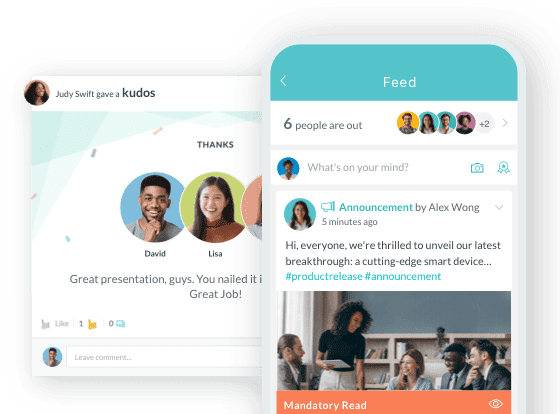
Workmates empowers employees to stay informed, connected, and appreciated—whether they’re on the front line, in the office, or remote. Recognition drives 12x higher engagement.Trusted by industry leaders in every sector




Cut Onboarding Costs by 60%.
Take the confusion and follow-ups out of onboarding with automated workflows, digital forms, and structured portals—so new hires ramp faster 3X quicker.Trusted by industry leaders in every sector